In 2012, the Regional Committee passed a resolution endorsing a proposed roadmap on strengthening health systems as a strategic priority, as well as necessary steps towards boosting universal coverage with quality health services at both the population and individual levels. The resolution was based on an in-depth analysis, conducted by the Regional Office in 2012, of the challenges facing health development in the Region and a review of WHO’s work in supporting Member States in addressing these challenges.
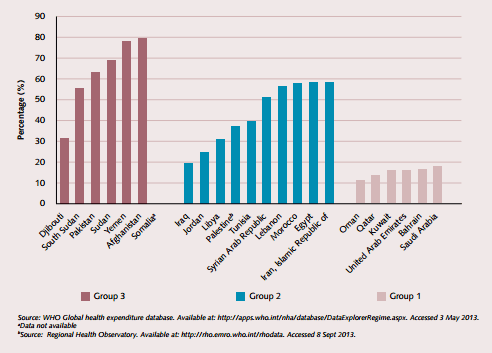
Health systems in the Region face many challenges that are generally cross-cutting in nature and apply to most countries irrespective of socioeconomic and health development. Addressing these challenges is critical to the achievement of universal health coverage. Countries have been categorized into three groups based on population health outcomes, health system performance and level of health expenditure (see Table 1)1. Countries in groups 2 and 3 face inadequate financing and a high share of out-of pocket expenditures for health. In some low-income countries, such payments are as high as 75% of the total health expenditure. High levels of out-of-pocket payment are a major impediment to the move towards universal health coverage (Figure 1). Other challenges relating to the lack of comprehensive, people-centred, and quality health care services, ensuring adequate health workforce, improving access to essential medicines and technologies and bridging the gaps that currently exist in health information systems will also have to be addressed in the journey to universal health coverage. The need for high-level political will and commitment to move towards universal health coverage with quality population and individual health services is the predominant challenge for many countries.
Table 1. Trends in key health outcomes in the Eastern Mediterranean Region, 1990–2010
|
Table 1. Trends in key health outcomes in the Eastern Mediterranean Region, 1990–2010* |
|||||||||
| Health status indicator |
Group 1 countries |
Group 2 countries |
Group 3 countries |
||||||
|
1990 |
2000 |
2010 |
1990 |
2000 |
2010 |
1990 |
2000 |
2010 |
|
|
Life expectancy at birth (years) |
72.6 |
74.1 |
75.0 |
69.2 |
71.2 |
73.4 |
52.8 |
56.6 |
60.2 |
|
Maternal mortality ratio (per 100 000 live births) |
24.0 |
18.0 |
17.0 |
115 |
79 |
63 |
750 |
625 |
360 |
|
Infant mortality rate (per 1000 live births) |
17.5 |
– |
8.5 |
36.5 |
– |
19 |
95.5 |
– |
71.5 |
|
Under 5 mortality rate (per 1000 live births) |
21.5 |
– |
9.5 |
45.5 |
– |
22 |
126.5 |
– |
97 |
|
Total fertility rate |
5.2 |
3.9 |
2.2 |
5.6 |
3.7 |
2.9 |
6.6 |
6.3 |
6.0 |
* Values are medians
– Information not available
Source: Health systems strengthening in countries of the Eastern Mediterranean Region: challenges, priorities and options for future action. Technical paper presented to the WHO Regional Committee for the Eastern Mediterranean, Fifty-ninth session, 2012 (available at www.emro.who.int/about-who/rc59/).
Figure 1. Share of out-of-pocket in total health expenditure by country group, 2011 (%)
Health financing and governance
WHO’s work in health financing was rejuvenated following the publication of the World Health Report 2010, which focused on reforming health financing systems to move towards universal health coverage. In 2012, requests were received from countries in all the three groups for support in this area. WHO has also focused on building the national capacities to generate the evidence needed to inform equitable, efficient and sustainable health financing policies. This included a capacity-building workshop in the new system of health accounts (SHA 2011) provided to health financing experts from 11 countries and a capacity-building exercise on the use of the new WHO tool OASIS (Organizational assessment for improving and strengthening health financing), aimed at assessing the bottlenecks undermining health financing systems performance. The Regional Office prioritized the assessment of progress towards universal health coverage in the Region. An assessment framework was developed and implementation is planned in 2013. This is intended to support Member States and WHO in monitoring equity in health financing and progress towards social health protection.
Two events provided opportunity for Member States to share experiences in reforming health financing systems to move towards universal health coverage: a policy dialogue between ministers of finance and health on “Value for money, sustainability and accountability in the health sector”, held in Tunisia for African Member States in collaboration with the African Development Bank and other development agencies; and a side session on health financing and universal health coverage, held during the 59th session of the Regional Committee. The two events have engaged countries in the current global debates around health care financing and its vital role in promoting the agenda of universal health coverage. The events were followed by a high-level seminar on health financing organized in Cairo in January 2013.
The purpose of employing the various health financing analytical tools is to generate results that can be used in national policy dialogues around the future of health financing in the specific local contexts. The Regional Office has facilitated such dialogues and focused discussions around health financing in Libya, Oman and Tunisia and provided technical support to other countries. The work to map health financing and assess where countries stand in terms of their health financing system goals and the move towards universal health coverage is progressing and has attracted the attention of a range of policy-makers.
The capacity of ministries of health in formulating and evaluating evidence-based policies and plans and in regulating the health sector is often inadequate and varies between countries. The engagement of key non-health sectors, which is essential in developing and implementing health policies as an integral part of national development plans, needs to be strengthened in almost all countries. Effective mechanisms need to be put in place for facilitating multisectoral action, based on international experience and lessons learned. The potential contribution of the private health sector to public health remains untapped. At the same time, the sector is not sufficiently regulated to ensure quality and prevent inappropriate practices. The private sector rivals the public sector in provision of primary health care services in several group 2 and 3 countries. However, its role is not well defined, its capacities poorly understood, and its practices not well monitored. Information is commonly lacking or insufficient about many of its functions, about the range of services it provides in different countries and about the financial burden to the users of these services. Based on resolution EM/RC59/R.3, a focus on the private sector has been included in the programme of work of the Regional Office in 2013.
In the area of governance, a number of advisory missions were undertaken. A multi-partner mission to Pakistan made recommendations to the Government following the decision to abolish the Ministry of Health and devolve the health sector to the provinces. An in-depth review of the health system in Morocco was undertaken following the recent constitutional amendment that recognized health as a human right, and a series of missions to Libya included an in-depth review of the health system and assessment of primary health care facilities and hospitals.
The work on health policy and governance also focused on capacity-building and country support in more than half of the countries of the Region. The health system profiles of four countries were updated and profiles of another four countries are in the process of publication.
Health information systems
The health information systems are generally weak in many countries and need to be improved, especially in quality and timeliness of reporting. There are important gaps in all countries of the Region. Data collection is fragmented and often duplicated and key areas related to monitoring of health status, health outcomes and health system performance are either missing or poorly integrated into the national health information system. More specifically, there are major gaps in reporting of cause-specific mortality and health facility records, in conducting regular health surveys, in routine and other data collection activities and in the availability of information disaggregated by age, gender, location and/or socioeconomic status; all coupled with a scarcity of human resources trained in epidemiology and health information systems. Important variations in regional and country estimates are also observed. In discussions with Member States, coordination and strengthening collaboration in the development and reporting of estimates emerged as key priorities and will receive focus in 2013.
The strengthening of capacity in health information is also important, for decision-making and developing and evaluating policies and plans. This was emphasized by the Regional Committee in resolution EM/RC59/R.3. Civil registration and vital statistics (CRVS) received special attention in 2012. Registration of births and deaths needs strengthening in almost all countries. A rapid assessment of CRVS systems was conducted to establish a baseline of the current situation and identify gaps and priorities for improvement. The results show that almost 40% of countries have either inadequate or weak systems, and only 25% have satisfactory systems. However, overall, these systems serve only 5.3% of the population in the Region. A satisfactory level of CRVS system reflects its ability to produce data of sufficient quality to adequately cover the needs for policy- and decision-making and for monitoring the impact of interventions and development programmes. These results have paved the way for conducting a comprehensive assessment, in collaboration with relevant partners and stakeholder, as a first step in the development of country action plans for CRVS.
The Regional Office launched a Regional Health Observatory, which is directly accessible through the regional web site, to support the dissemination and use of health information. This is now the main source for country health-related information, drawing on more than 40 databases and 800 indicators collected since 1990.
WHO’s work in 2013 will aim to develop technical guidance on the essential elements of health information systems, including consensus on a core list of indicators covering health risks and determinants, health outcomes (morbidity and mortality) and health system performance.
Health workforce development
Most countries need to develop a balanced, motivated, well-distributed and well-managed health workforce with the appropriate skills mix. The overall workforce density in the Region is below the global average of 4 skilled health workers per 1000 population. Eight countries (Afghanistan, Djibouti, Iraq, Morocco, Pakistan, Somalia, Sudan and Yemen) are classified as facing a crisis in human resources for health, largely due to insufficient measures to facilitate market entry, such as lack of preparation of the workforce through strategic investment in education and effective and ethical recruitment practices. Another challenge is inadequate workforce performance due to lack of adequate continuing education and training, as well as poor management practices in the public and private sectors. Policies for retention of health workers and for managing migration and attrition to reduce wasteful loss of human resources are also lacking, despite the magnitude of the problem.
There are serious challenges to ensuring access to quality nursing education in the Region, in particular inadequate investment and the low priority given to nursing education; lack of capacity in nursing schools in terms of the availability of trainers as well as infrastructure; the need to further update nursing curricula in order to bridge the service–education gap; the limited institutional capacity to offer post-basic training programmes; and inadequate emphasis on continuous professional development programmes.
Human resources observatories in Afghanistan and Palestine were set up to support health workforce development. The Regional Office has promoted several regional tools to strengthen the capacity for workforce governance and planning, such as a guide for accreditation of health professions programmes, and tools to optimize staff workload in health facilities and to make workforce projections.
Initiatives to strengthen nursing and midwifery training included support to several countries in developing their national strategic plans. The leadership and management training programme, developed by the International Council of Nurses with WHO support, continued in several countries.
All countries are currently facing some gaps in health workforce development, mainly in the areas of production, distribution, training and continuing education, and retention, although the type and magnitude varies between countries. Addressing these gaps and developing effective and feasible strategies in these areas will require an in-depth review and analysis of existing regional and international experience and lessons learned. Health workforce development is an areas that will require greater attention in the next two years.
Integrated service delivery
Many countries are making efforts to establish effective family practice programmes as the principal vehicle for delivering primary health care and increasing access and coverage of population to health care services. Family practice is an overarching model of care delivery that contributes to moving toward universal health coverage. The challenges include the lack of adequately trained family physicians, nurses and other practitioners, maldistribution of the health workforce and insufficient engagement with hospitals to provide the necessary back-up and support.
There is a need to review international and regional experience and lessons learned based on workable models of family practice and develop guidance on feasible strategies to strengthen family practice in the Region and these areas will be the focus of attention in the coming period.
Patient safety and health system strengthening component of the global health initiatives
Support for patient safety continued with the expansion of the Patient Safety Friendly Hospital Initiative to more countries. The patient safety assessment manual was translated into Arabic and the second edition is being finalized. The patient safety multi-professional curriculum guide developed by WHO was launched; several medical schools have started to integrate it in the training curricula. Work is under way to develop a patient safety improvement toolkit that includes practical steps and needed actions for building a comprehensive patient safety improvement programme.
System-wide barriers, relating to accessibility, availability and affordability of health care, are a substantial challenge to the implementation of public health programmes, affecting the provision of services and reducing programme performance. Poor health system performance is also a constraint. In the area of health system management, a study on decentralization in 10 countries and another study on hospital management and performance assessment in 12 countries were conducted and the results shared.
Several Member States have benefited from the health system strengthening component of the global health initiatives, e.g. GAVI Alliance, Global Fund to Fight AIDS, Tuberculosis and Malaria and International Health Partnerships Plus (IHP+). Over a five-year period, funds provided by the GAVI Alliance for strengthening health systems totalled US$ 160 million and by the Global Fund US$120 million. In most countries these funds are largely channelled through national governments, with technical support provided by WHO in the development of proposals for new rounds of funding, implementation monitoring and capacity-building. Countries that have used these funds well have demonstrated good progress towards health system strengthening. However, performance varies across countries and use of the funds is sometimes caught up in extensive government procedures. Three countries have also signed the IHP+ compact. This is not a funding initiative but encourages countries and partners to agree on one national health plan. There is variation in the extent to which the countries have shown commitment to IHP+.
Many countries in the Region face complex emergencies and most health systems are not well prepared to respond to these situations and are not resilient in extended emergencies. These countries need to be supported to enhance their collaboration, coordination, planning, communications and information exchange capacities.
Essential medicines and technologies
There is insufficient access to essential technologies (medicines, vaccines, biological and medical devices) in most countries in groups 2 and 3 and irrational use is common. While almost all countries have national regulatory authorities, performance needs to be improved. Most authorities focus on the regulation of medicines and not on the regulation of biological products, medical devices and clinical technologies including laboratories. Quality management, monitoring the private sector, and protecting public goods from commercial interests are weak and require attention.
In the area of essential technologies, six pharmaceutical country profiles were developed, national medicine policy documents were updated for two countries and five additional countries joined the good governance for medicines programme. National transparency assessment reports on vulnerability to corruption in the pharmaceutical sector were drafted for three countries and support was provided to more than 10 national regulatory authorities on good manufacturing practice inspections.
Capacity-building was supported in order to strengthen coordination between policy-makers and regulators on the proper use and evaluation of vaccines, such as diphtheria-tetanus-pertussis (DTP) and DTP-combo vaccines, as well as vaccine safety systems. Afghanistan, Sudan and Yemen received support to enhance their vaccine pharmacovigilance systems.
In the area of health technology and medical devices, missions to assess health technology infrastructure and management were conducted in several countries. In collaboration with WHO headquarters, a second wave of the global survey on medical devices was launched. Over 70% of Member States participated in this round compared to 40% in the first one. Results indicated that only 5% of the Member States of the Region have established policies and coordination units for medical devices, 29% have regulation and inventory systems and 16% have developed national procurement and maintenance guidelines. An intercountry consultation in this area of work will be organized in 2013.
1. Group 1: Bahrain, Kuwait, Oman, Qatar, Saudi Arabia, United Arab Emirates; Group 2: Egypt, Islamic Republic of Iran, Iraq, Jordan, Lebanon, Libya, Morocco, Palestine, Syrian Arab Republic, Tunisia; Group 3: Afghanistan, Djibouti, Pakistan, Somalia, South Sudan, Sudan, Yemen