Case report
G. Sadeghian,1 H. Ziaei,1 L. Shirani-Bidabadi1 and M.A. Nilforoushzadeh1
1Skin Disease and Leishmaniasis Research Center, Isfahan University of Medical Sciences, Isfahan, Islamic Republic of Iran (Correspondence to G. Sadeghian:
EMHJ, 2010, 16(3):344-345
Introduction
Lupoid leishmaniasis, a clinical form of cutaneous leishmaniasis, was described by Christopherson in 1923 [1]. It is a chronic condition that typically follows acute cutaneous leishmaniasis infection. In this clinical form, 1 to 2 years after healing of the acute lesion, new papules and nodules appear at the margin of the remaining scar. The papules have a granulomatous, lupoid appearance and are often associated with scaling. They characteristically present at the margin of the scarred area. Less commonly lesions may present months or years after the acute lesion has healed [2]. Most reported cases are associated with old world strains of leishmaniasis and Leishmania tropica is responsible for the majority of such cases [3]. The incidence of lupoid leishmaniasis has been reported in previous studies to range from 0.5% to 6.2% [4,5].
Histological features of this condition include well-organized epithelioid granulomas, surrounded by lymphocytes, amastigotes are absent and culture for leishmaniasis is frequently negative [4]; however, the leishmanin test is usually positive [5].
Lupoid cutaneous leishmaniasis is prevalent in endemic area of leishmaniasis, particularly in the Middle East and Afghanistan [6]. In this report we describe 2 cases of lupoid leishmaniasis that were not diagnosed for several years and caused large scars on the face.
Case reports
Case 1
A 17-year-old Afghan man presented to the Skin Disease and Leishmaniasis Research Center (SDLRC) in 2007 with 2 large atrophic plaques on both sides of his face and 1 on his right ear. He had been infected with cutaneous leishmaniasis in Afghanistan 10 years before but some red infiltrative nodules appeared at the margin of the remaining scars 2 years before referring to our centre (Figure 1). He complained of new lesions at the margin of the old scars which were progressing.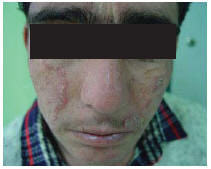
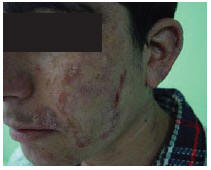
Figure 1 Patient 1 showing large atrophic plaques on both sides of his face. There were some red infiltrative nodules at the margin of the lesions.
Direct smear was negative for Leishman bodies, leishmanin test was positive (8 mm induration) and Mantoux test was negative.
Polymerase chain reaction (PCR) was used to identify the Leishmania species, which was found to be L. major. The patient, who had not previously undergone any treatment for cutaneous leishmaniasis, was treated with systemic meglumine antimoniate (Glucantime, Aventis, France) 20 mg/kg per day intramuscularly for 20 days. His response to this treatment was good and the marginal nodules disappeared (Figure 2). The patient was followed up for 1 year and showed no sign of recurrence.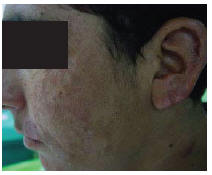
Figure 2 Patient 1 after treatment
Case 2
A 19-year-old Afghan man presented in 2007 with a large atrophic scar on one side of his face and nose. There were some red infiltrative nodules at the margin of the lesion which had appeared 3 years before referring to the SDLRC (Figure 3).The patient complained of recurrence and progression of his disease.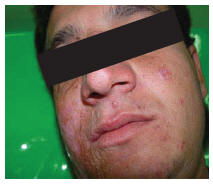
Figure 3 Patient 2 showing large atrophic scar on one side of his face and nose with red infiltrative nodules
Direct smear was negative for Leishman bodies and histological examination showed epidermal hyperplasia, severe infiltration of lymphoplasma cells and epithelioid granuloma without caseous necrosis or Leishman bodies. Leishmanin test was positive (10 mm induration) and Mantoux test was negative. L. major was identified using PCR.
This patient had also not been treated for leishmaniasis before and was treated similarly with systemic meglumine antimoniate (Glucantime, Aventis, France) 20 mg/kg per day intramuscularly for 20 days. His response to treatment was also good and the marginal nodules disappeared (Figure 4). He too was followed for 1 year and showed no sign of recurrence.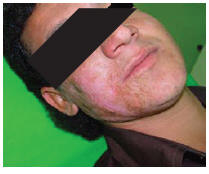
Figure 4 Patient 2 after treatment
Discussion
Lupoid leishmaniasis, also known as chronic or relapsing leishmaniasis, is widespread in the Middle East, where it represents up to 5% of all cutaneous leishmaniasis cases [7]. Although not as destructive as lupus vulgaris, lupoid leishmaniasis may persist and spread slowly for many years [8].
The clinical and histopathological features closely resemble lupus vulgaris, leading to diagnostic difficulty in distinguishing between these 2 conditions. Differential diagnosis is difficult and may depend on the detection of a few leishmania amastigotes in the histological sections, the growth of the promastigotes in cultures, or the identification of amastigotes by other techniques. PCR has been used to detect leishmania amastigote DNA in tissue samples obtained from patients with chronic lupoid leishmaniasis [5].
In a study in the Islamic Republic of Iran, L. major was identified in 63 patients with chronic lupoid leishmaniasis [9]. In our 2 reported cases, the patients had not been diagnosed despite having had the condition for several years because direct smears were negative. The delay in the diagnosis led to progression of the lesions, which caused the large scars on their faces. It was the use of PCR that allowed us to establish the diagnosis and identify the parasite responsible for the lesions as L. major. Both the patients were successfully treated with systemic meglumine antimoniate.
We recommend that the diagnosis of lupoid leishmaniasis be considered in all patients from endemic areas of leishmaniasis who present with chronic lesions, especially with facial lesions. Although cutaneous leishmaniasis is self-limiting, if the lupoid form of cutaneous leishmaniasis is left untreated, it will progress and destroy the skin leading to large scars. Early diagnosis and treatment are vitally important to prevent this complication.
References
- Christopherson JB. Lupus leishmaniasis: a leishmaniasis of the skin resembling lupus vulgaris: hitherto unclassified. British journal of dermatology, 1923, 35:123–31.
- Bowling JCR, Vega-Lopez F. Clinicopathological case. Clinical and experimental dermatology, 2003, 28(6):683–4.
- Asillian A et al. Carbon dioxide laser for the treatment of lupoid cutaneous leishmaniasis (LCL): A case series of 24 patients. Dermatology online journal, 2006, 12(2):3.
- Nilforoushzadeh MA et al. The therapeutic effect of combined cryotherapy, paramomycin, and intralesional meglumine antimoniate in treating lupoid leishmaniasis and chronic leishmaniasis. International journal of dermatology, 2006, 45(8):989–91.
- Aradeh S et al. Studies on chronic (lupoid) leishmaniasis. Annals of tropical medicine and parasitology, 1980, 74(4):439–45.
- Gurel MS, U Lukanligil M, Ozbilge H. Cutaneous leishmaniasis in Sanliurfa: epidemiologic and clinical features of the last four years (1997–2000). International journal of dermatology, 2002, 41(1):32–7.
- Paradisi M et al. Un caso di leishmaniosi lupoide in eta pediatrica diagnostica mediante PCR [A pediatric case of lupoid leishmaniasis diagnosed by PCR]. Minerva pediatrica, 2001, 53(1):33–7.
- Even-Paz Z, Sagher F. Some basic medical problems illustrated by experiments with cutaneous leishmaniasis. South African medical journal, 1961, 35:565–81.
- Momeni AZ et al. Chronic lupoid leishmaniasis. Evaluation by polymerase chain reaction. Archives of dermatology, 1996, 132(2):198–202.








