C. Bodenschatz,1 M. Talaat,1 A. Kandeel,2 A.L. Lohiniva,1 E. Radwan1 and F. Mahoney1
أنماط وصف الـحُقَن في مرافق الرعاية الصحية في القطاع العام في مصر
كارولين بودينشاتز، مها طلعت، عمرو قنديل، أنالينا لومينيفيا، إيمان رضوان، فرانك ماهوني
الخلاصـة: تقيِّم هذه الدراسة تكرار استخدام الـحُقَن والأساس المنطقي له في مرافق الرعاية الصحية في مصر، استناداً إلى المؤشِّرات الأساسية لمنظمة الصحة العالمية لاستخدام الأدوية. وقد راجع الباحثون 1406 وصفة دوائية في 43 مستشفى تم اختيارها عشوائياً، إلى جانب عيادتين للرعاية الصحية الأولية في محافظتين في صعيد مصر (مصر العليا) وفي شمال مصر (مصر الدنيا)، وذلك عام 2001. ووجد الباحثون أن المرضى يتلقون حقنة كل 18.1 مقابلة لهم، أما أكثر الأدوية التي توصف حَقْناً فكانت مضادات العدوى (%56.9 من الـحُقَن) والمسكِّنات (%13.7). وتوصف الـحُقَن بتواتر أعلى في المستشفيات منه في عيادات الرعاية الصحية الأولية، وفي المواقع الريفية أكثر مما في المواقع الحضرية. ويمكن استبدال معظم الـحُقَن (%94.7 منها) بمستحضرات فموية. والحاجة ماسة إلى بذل جهود إضافية لتفعيل برنامج الأدوية الأساسية في مصر لتحسين الوصف الرشيد للأدوية.
ABSTRACT This study assessed the frequency of and rationale for use of injections at health care facilities in Egypt based on WHO core drug use indicators. We reviewed 1406 prescriptions in 43 randomly selected hospitals and primary health care clinics in 2 governorates in Upper and Lower Egypt in 2001. Patients received an injection at 18.1% of encounters. The most frequently prescribed parenteral drugs were anti-infectives (56.9% of injections) and analgesics (13.7%). Injections were more often prescribed in hospitals than in primary health care clinics and in rural than in urban settings. Most injections (94.7%) could have been replaced by a suitable oral preparation. Further efforts are needed to enforce the essential medicines programme in Egypt to improve rational drug prescribing.
La prescription d’injections dans les établissements de soins de santé publique en Égypte
RÉSUMÉ Cette étude a évalué la fréquence et les raisons de l’utilisation des injections dans des établissements de soins de santé en Égypte, sur la base des indicateurs fondamentaux de l’utilisation des médicaments définis par l’OMS. Nous avons examiné 1 406 ordonnances établies dans 43 hôpitaux et centres de soins de santé primaires choisis au hasard dans deux gouvernorats de Haute et de Basse-Égypte en 2001. Les patients ont reçu une injection lors de 18,1 % des consultations. Les médicaments parentéraux les plus fréquemment prescrits étaient des anti-infectieux (56,9 % des injections) et des analgésiques (13,7 %). Les injections étaient plus souvent prescrites en milieu hospitalier que dans les centres de soins de santé primaires, et dans les zones rurales que dans les zones urbaines. La plupart des injections (94,7 %) auraient pu être remplacées par une préparation orale adaptée. Il est nécessaire de poursuivre les efforts visant à faire appliquer le programme des médicaments essentiels en Égypte afin d’encourager l’usage rationnel des médicaments.
1Infection Control Unit, US Naval Medical Research Unit No. 3, Cairo, Egypt (Correspondence to C. Bodenschatz:
2National Infection Control Programme, Ministry of Health and Population, Cairo, Egypt.
Received: 06/08/07; accepted: 04/10/07
EMHJ, 2009, 15(6):1440-1448
Introduction
The overuse of injections to administer medication is common in many countries where there is a preference for injections among health care workers and patients [1]. Studies among patients seeking care in outpatient settings in developing countries indicate that more than half are treated with injections, of which over 90% may be unnecessary or could be provided in an oral formulation [2]. Antibiotics, vitamins or analgesics are commonly prescribed by injection for upper respiratory tract infections, diarrhoea, fever or general fatigue [3].
The reasons for popular demand for injections include beliefs that injections are a “stronger” medication [4], work faster [unpublished data, Centers for Disease Control, 1998] and are a more advanced technology [5]. Among health care workers, motivations for use of injections include belief in the greater efficacy of injected drugs [6], ability to ensure compliance with treatment and financial incentives. In Egypt, injections are the preferred mode of treatment by both patients and prescribers [7]. A community-based study in Egypt revealed a higher average number of injections per person per year (4.2) compared with other low-income countries (3.4, range 1.7–11.3) [8,9].
The high prevalence of hepatitis C virus (HCV) infection in Egypt has recently been attributed to unsafe injections [10,11]. It has been hypothesized that wide-scale transmission of HCV occurred between the 1960s and 1980s during mass campaigns to treat schistosomiasis [10–12]. Although those treatment campaigns were discontinued 2 decades ago, high rates of HCV infection are still observed in all age groups of the Egyptian population, indicating that other risk factors are responsible for the sustained transmission [7].
This report provides results from a study to evaluate the frequency and type of injections prescribed in public health care facilities in 2 governorates in Egypt. The objectives of the survey were to examine the extent to which injections are prescribed at the dispensary level in public health care facilities and to evaluate the necessity of prescribed injections by medical condition.
Methods
The study was conducted in urban and rural areas of 2 governorates of Egypt: Sharqiyah (Lower Egypt) and Qena (Upper Egypt) during April and May 2001. Data were collected in the outpatient department of government hospitals and primary health care clinics.
Data collection
Information was collected through record review and patient interviews in 43 facilities (21 hospitals and 22 primary health care clinics) randomly selected from an enumerated list of all 196 government hospitals and primary health care clinics in the 2 governorates (Table 1). From each health care facility, 30 medical encounters from clinic registers of the previous day were randomly selected by systematic sampling. Additionally, 20 encounters were reviewed prospectively using a patient interview to collect information on injections prescribed in a medical encounter on the day of the interview.
The project team developed a set of quantitative drug use and prescribing indicators using World Health Organization (WHO) reference materials [13]. For each prescription examined, the following details were recorded on a structured data collection form: name of each drug, patient number, route of administration, specified condition (if available) and patient’s age and sex.
Study personnel
Egyptian physicians interested in drug use issues were recruited from the Ministry of Health and Population Field Epidemiology Training Programme to collect data for the survey. The interviewers participated in a 1-day in-service training on the basic elements of drug use indicators and the use of the data collection instruments. They performed a series of pilot interviews and assessments to standardize data responses. One trained interviewer collected data from each health facility over a period of 1 day per facility.
Data analysis of patient register
The survey data were entered into a computerized database. Descriptive analysis was performed to evaluate prescribing practices by location and to compare prescribing practices between different sources of health care services. Coding frames were developed for the analysis of the data. Drugs were coded according to therapeutic groups as listed in the International Anatomical Therapeutic Chemical Classification System (ATC). Those drugs which had more than 1 therapeutic indication were coded according to their most common use. Penicillins, other anti-infective agents (including sulfa drugs), anti-infective dermatological drugs, anti-infective ophthalmologic agents and antidiarrhoeal drugs with streptomycin, neomycin, nifuroxazide were regarded as anti-infectives; antiamoebic, antigiardiasis and antihelminthic drugs were not regarded as anti-infectives but classified as gastrointestinal drugs. Vaccines were excluded [13].
Diagnoses were coded according to the WHO group classification model of diseases, clinical indications and symptoms (WHO EMLib). Medical conditions were recorded wherever information was available. For each stated condition, injections were classified as “avoidable” when there was an oral alternative according to drug therapy recommended in standard medical texts [14].
Results
Overall, in 255 out of 1406 encounters (18.1%) patients were prescribed at least 1 injection (range 1–3 injections per encounter). In 1.4% of encounters patients received more than 1 injection. Residents of Upper Egypt were more likely to have an injection prescribed (20.1% of encounters) compared with those living in Lower Egypt (16.4%). Often injections were combined with oral medication. The age-specific rate of encounters including at least 1 injection was highest in encounters with patients aged 41–50 years (mean 28%) and lowest among those aged 21–30 years (mean 14%) (Figure 1). The mean rate of encounters with at least 1 injection was 19.0% in females and 16.8% in males.
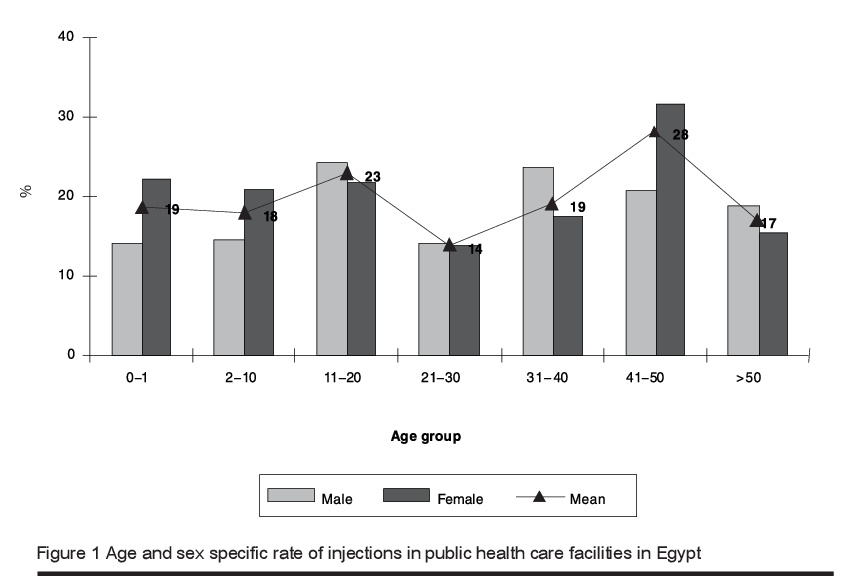
Patients who received services in the outpatient department of a hospital were more likely to be prescribed an injection compared with those visiting a primary health care clinic (21.7% versus 13.1% of encounters) (Table 2). Injections were particularly common in rural hospitals (34.1%). When analysed by location, the frequency of encounters with an injection was higher in rural than in urban settings (25.4% versus 13.9%) (Table 2).
Among the main anatomical groups, anti-infectives were the most common injections prescribed. They were used in 56.5% of encounters, followed by parenteral analgesics (13.7%) (Table 3). Penicillins accounted for 71/255 injections prescribed (27.8%), followed by ampicillin (11.8%), dipyrone (5.5%) and amoxicillin (5.1%). Of the 71 injections for penicillins, procaine penicillin G accounted for 58.2%, followed by long-acting penicillin (18.9%). When analysed by the stated diagnosis, 47.8% of the 138 parenteral antibiotics were prescribed for respiratory tract infections followed by 10.9% for dental care purposes.
Overall, 160/160 (94.7%) of all injections prescribed for a specific medical condition were judged to be avoidable, i.e. could have been replaced by an equivalent oral preparation or substituted with another oral drug. Therapeutic indications where an injection was the only suitable preparation or could not be substituted by an alternative oral agent included: postnatal vaginal bleeding (methylergometrine maleate) and diabetes mellitus type I (insulin) (Table 4).
Discussion
This is the first study that describes the extent and characteristics of injections prescribed in outpatient settings in government health care facilities in Egypt. The information gained from the study serves as the baseline for measuring the effectiveness of interventions undertaken to promote rational use of injections among prescribers and consumers.
Our findings are consistent with other studies in developing countries demonstrating that too many injections are prescribed in outpatient settings than are medically justified. The frequency of prescribing injections ranges from 17% to 80% in studies conducted in Ethiopia, Ghana, Morocco, Pakistan, Tanzania and Zimbabwe [15–19].
The popularity of injections among the Egyptian population has been widely reported [9]. In this study, we found that injections were particularly popular in rural areas. Cultural differences and different education levels between urban and rural residents in Egypt may lead to different perceptions or beliefs attributed to the power of injections which may influence the demand for injections [20]. Doctor–patient relations might also differ. Frequent change of shifts and the much higher numbers of doctors working in urban health settings result in different doctor–patient relations than rural areas, which might influence prescribing. In rural areas in Egypt, medical doctors are permitted to have private clinics in the afternoon in addition to their government position in public health care facilities. Therefore, prescribing injections may increase patients’ satisfaction and bring the patient back to the doctor’s private clinic and/or increase his reputation as a “good doctor” in the village. However, a more detailed qualitative and quantitative insight into the variability of actual drug prescribing between rural and urban areas in Egypt is needed.
In this study, we concluded that 94.7% of injections performed in the outpatient settings were unnecessary and could have been effectively replaced by suitable oral preparations indicated for the same medical condition. In general, parenteral therapy should be reserved for severe infections generally associated with hospitalization. This judgement might raise issues for discussion as clinicians may have valuable reasons for prescribing injections, even in an outpatient setting. In a setting of poor compliance, long-acting penicillin may be indicated to ensure compliance with treatment. Nevertheless, patient exposure to parenteral anti-infective drugs appears to be very high in Egypt. New oral agents, e.g. fluoroquinolones and cephalosporins, are available on the market that have demonstrated similar efficacy to parenteral therapy in patients with pneumonia, urinary tract infections, skin and soft tissue infections, osteomyelitis and bacteraemia [21]. Intravenous formulations are more expensive than the equivalent oral formulations, and the preparation and administration of intravenous drugs adds significant additional costs [22].
Additional issues of concern in Egypt are the indiscriminate and inappropriate use of anti-infective drugs, regardless of the mode of delivery. For example, in this study many anti-infectives were prescribed for respiratory tract infections even though most of these infections were likely to be viral in etiology. Diagnoses that warrant antimicrobial therapy are, for example, community-acquired pneumonia, bacterial sinusitis and selected cases of acute exacerbations of chronic bronchitis. The efficacy of antibiotics to treat otitis media with effusion, acute bronchitis and rhinitis is not well established [23]. Studies conducted among family practice providers in the United States of America revealed that 79% of antibiotic prescriptions to treat respiratory tract infections were unnecessary [24]. Awareness of clinical manifestations that help to differentiate viral from bacterial infection and the use of treatment guidelines can promote the appropriate management of respiratory tract infections and rationalize the use of anti-infectives [23].
Any drug utilization study based on the WHO core drug use indicators has limitations. Determining the quality of diagnosis and evaluating the adequacy of drug choice is beyond the scope of the prescribing indicators [13]. We therefore had to accept the diagnosis or conditions stated as the starting point in assessing the appropriateness of the prescribed injections. The data for this study were from 2001. However, it is the first study that describes the extent and characteristics of injections prescribed in outpatient settings in government health care facilities in Egypt.
Recommendations
This study established standard reference data on injection prescribing indicators, as well as on related injection use parameters, and identified priority areas for intervention. However, further studies to elaborate and strengthen the observations made are also recommended.
Interventions to improve drug use should be designed to bring about changes in behaviour. A suggested starting point is to establish Hospital Drug and Therapeutics Committees to act as “agents of change”. Their main role is to optimize rational drug use by evaluating the clinical use of drugs, developing policies for drug use and administration and managing the formulary system. Public education about medicines and continuing in-service education programmes for health care workers at all levels will help to improve rational drug prescribing. As irrational use of drugs is not only widespread in public health settings, the private sector should be addressed as well. Continuous monitoring of drug utilization is strongly recommended by WHO.
Acknowledgements
The authors thank all health officials in Sharqiyah and Qena governorate, those who helped in collecting the data, and Stephen Luby for his kind support and for reviewing the manuscript.
This work was supported by USAID, Work Unit No. 80000.000.000. E0022. The views expressed in this article are those of the authors and do not necessarily reflect the official policy or position of the Department of the Navy, Department of Defense, the US Government, nor the Egyptian Ministry of Health and Population.
This research was supported in part by an appointment to the Research Participation Program at the Centers of Disease Control and Prevention, National Center for Infectious Disease, Division of Bacterial and Mycotic Diseases, administered by the Oak Ridge Institute for Science and Education through an interagency agreement between the U.S. Department of Energy and CDC. 111310 ORISE fellow.
This work was prepared as part of the principal author’s official duties for the US Government. Title 17 USC §105 provides that “Copyright protection under this title is not available for any work of the United States Government”. Title 17 USC §101 defines a US Government work as a work prepared by a military service member or employee of the US Government as part of that person’s official duties.
The study protocol was approved by the US Naval Medical Research Unit No. 3 Institutional Review Board (Protocol # CPHS 108 DOD 31900) and work is conducted in compliance with all Federal regulations governing the protection of human subjects.
References
- Safety of injections: a brief background. Fact sheet No. 231, October 1999. World Health Organization [website] (http://www.who.int/injection_safety/toolbox/en/InjectionFactSheet2002.pdf, accessed 15 June 2009).
- Holloway K. Safe Injection Global Network (SIGN). Annual meeting report: 24–25 October 2002. Geneva, World Health Organization, 2002 (WHO/BCT/02.13).
- Simonsen L et al. Unsafe injections in the developing world and transmission of bloodborne pathogens: a review. Bulletin of the World Health Organization, 1999, 77(10):789–800.
- Luby SP et al. The relationship between therapeutic injections and high prevalence of hepatitis C infection in Hafizabad, Pakistan. Epidemiology and infection, 1997, 119:349–56.
- Reeler AV. Injections: a fatal attraction? Social science and medicine, 1990, 31(10):1119–25.
- Safe Injection Global Network (SIGN). Initial meeting report, October 4–5, 1999. Geneva, World Health Organization, 2000 (WHO/DCT/00.1).
- Wasley A, Alter MJ. Epidemiology of hepatitis C: geographic differences and temporal trends. Seminars in liver disease, 2000, 20(1):1–16.
- Lohiniva AL et al. Therapeutic injections in the context of Egyptian culture. Promotion and education, 2005 12:13–8.
- Talaat M et al. Overview of injection practices in two governorates in Egypt. Tropical medicine and international health, 2003, 8(3):234–41.
- Frank C et al. The role of parenteral antischistosomal therapy in the spread of hepatitis C virus in Egypt. Lancet, 2000, 355:887–91.
- Rao MR et al. Further evidence for association of hepatitis C infection with parenteral schistosomiasis treatment in Egypt. BMC infectious diseases, 2002, 2(1):29.
- Barnard H. Hepatitis C in Egypte, een iatrogene epidemie [Hepatitis C in Egypt, an iatrogenic epidemy]. Nederlands tijdschrift voor geneeskunde, 2000, 144(49):2378.
- International Network for Rational Use of Drugs and World Health Organization. How to investigate drug use in health facilities: Selected drug use indicators. Geneva, World Health Organization, 1993 (EDM Research Series No. 7; WHO/DAP/93.1).
- Beers MH, Berkow R. Merck manual of diagnosis and therapy, 17th ed. New York, John Wiley and Sons, 1999.
- Desta Z et al. Assessment of rational drug use and prescribing in primary health care facilities in North West Ethiopia. East African medical journal, 1997, 74:758–63.
- Bosu WK, Ofori-Adjei D. An audit of prescribing practices in health care facilities of the Wassa West district of Ghana. West African journal of medicine, 2000, 19:298–303.
- Simon N et al. Prescription et utilisation des medicaments au Maroc [Drug prescription and utilization in Morocco]. Thérapie, 1998, 53:113–20.
- Najmi MH et al. Prescribing practices: an overview of three teaching hospitals in Pakistan. Journal of the Pakistan Medical Association, 1998, 48:73–7.
- Massele AY, Nsimba SE, Rimoy G. Prescribing habits in church-owned primary health care facilities in Dar Es Salaam and other Tanzanian coast regions. East African medical journal, 2001, 78:510–4.
- EI-Zanaty F, Way AA. Egypt interim demographic and health survey 2003. Cairo, Ministry of Health and Population, National Population Council, El-Zanaty and Associates and ORC Macro, 2004.
- Craig WA, Andes DE. Parenteral versus oral antibiotic therapy. Medical clinics of North America, 1995, 79 (8):497–508.
- Davey P, Parker S. Cost effectiveness of once-daily oral antimicrobial therapy. Journal of clinical pharmacology, 1992, 32:706–10.
- File TM Jr, Hadley JA. Rational use of antibiotics to treat respiratory tract infections. American journal of managed care, 2002, 8(8):713–27.
- Scott JG et al. Antibiotic use in acute respiratory infections and the ways patients pressure physicians for a prescription. Journal of family practice, 2001, 50:853–8.








