In 2018, WHO's Regional Office for the Eastern Mediterranean continued to support its Member States in containing outbreaks and building country capacities in prevention and surveillance of, preparedness for, and response to health threats posed by emerging and re-emerging infectious diseases.
The Infectious Hazard Management programme of the Department of Health Emergencies in the Eastern Mediterranean Region worked closely with Member States to:
respond to and contain a number of outbreaks of high-threat pathogens, including MERS in Saudi Arabia and Kuwait, cholera in Yemen and Somalia, Crimean-Congo haemorrhagic fever in Afghanistan and Iraq, extensive drug resistant typhoid fever in Pakistan, chikungunya and Acute Watery Diarrhoea in Sudan, dengue fever in Oman, West Nile fever in Tunisia and many more;
expand the Emerging and Dangerous Pathogen Laboratory Network (EDPLN);
Strengthen surveillance systems for detection of high-threat pathogens in Djibouti, Libya, occupied Palestinian territory, , Somalia, Sudan, Syria, and Yemen.
The following photo essay covers some of the major public health activities undertaken this year in support of Ministries of Health, in coordination with regional and global health partners.

Pandemic and epidemic diseases: 2018 in retrospect
A 6-year-old girl in Hudaydah shows her oral cholera vaccination card (Photo: WHO/Sadeq Al-Wesabi).
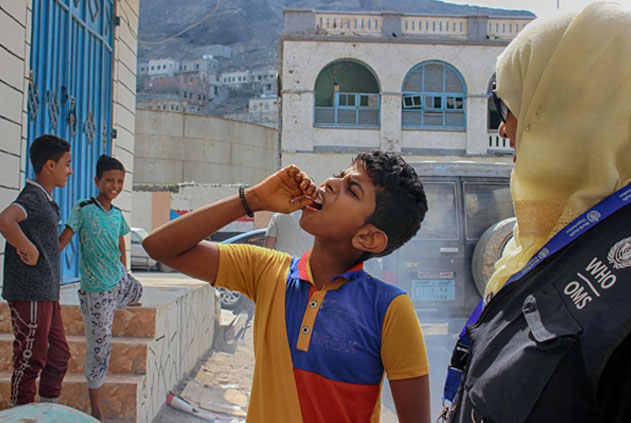
Cholera in Yemen
In 2018, the cholera outbreak in Yemen became the largest in human history, with over 1,3 million cases and over 3000 deaths.
Throughout the year, WHO, in coordination with Health and WASH cluster partners, continued to support the Ministry of Public Health and Population of Yemen to contain this outbreak through the strengthening of disease surveillance, case management, administering oral cholera vaccine, and improved access to safe water and sanitation.

Chikungunya and Acute Watery Diarrhoea in Sudan
Sudan continued responding to the outbreak of acute watery diarrhoea, including by supporting access to safe water (as pictured), resulting in fewer new cases and deaths in 2018.
However, the country faced a new challenge in May, when an outbreak of chikungunya spread rapidly through the north-eastern part of the country, mainly in the state of Kassala, infecting over 20 000 people. Further complicating the outbreak were coinfections with dengue, which made diagnosis more difficult since the symptoms of both diseases overlap.
In response, Sudan’s Health Ministry lead response activities with the support from WHO and other partners, including aggressive vector control, risk communication to reduce the risk of infection, and enhancing the surveillance system. The outbreak was effectively contained by November.

Pandemic Influenza Preparedness training in Tunisia
During a three-day workshop held in Tunis in August, Ministry of Health staff from Morocco, Tunisia, Oman, Tanzania and Ghana joined experts from WHO and developed a tool to identify and fill gaps in their National Pandemic Influenza Preparedness Plans.
Participants focused on improving influenza surveillance, risk assessment and determining severity of an outbreak. Furthermore, participants learned about maintaining essential health services in the event of a pandemic, as well as clinical management, prevention, risk communication, and testing and revising of plans.

Somalia rolls out electronic system for Early Warning Alert and Response Network (EWARN)
To help Somalia improve the real-time detection of and response to health threats across the country, IHM organized a four-day training workshop on the use of the newly updated electronic platform for disease early warning systems, called Early Warning Alert and Response Network (EWARN).
Health surveillance officers from 11 regions in Somalia received training on epidemic disease surveillance and response, alert verification, rapid response activities, and reporting of alerts to capture, analyse, and share data in real-time using web-based platforms, mobile networks and smart technologies.

Hajj 2018: another outbreak-free event
During the second half of August, 2.7 million muslim pilgrims assembled in the holy sites of Saudi Arabia for the annual Hajj. The combination of a high-threat disease like Middle East Respiratory Syndrome and a large congregation of pilgrims in the same place at the same time have made the event a very high-risk situation since the emergence of the disease in 2012.
WHO supported the Saudi Arabia’s Ministry of Health with necessary technical assistance on assessing and implementing necessary public health preparedness and readiness measures as required under the International Health Regulations (2005) for mass gathering events.
By implementing the appropriate public health measures, WHO and Saudi’s Health Ministry kept the Hajj free from any public health event of potential concern once again this year - as it has done since the emergence of MERS in 2012.

Rapid Response Teams trained across the region
WHO conducted trainings for multidisciplinary Rapid Response Teams (RRTs) focused on Ebola and MERS in Pakistan, Saudi Arabia, Sudan, and Libya, with another training being prepared in Somalia. Over 130 team members received training on topics like rapid risk assessment, outbreak investigation, epidemiological data analysis, and implementing initial public health measures to contain and limit the spread of an outbreak.
Furthermore, national RRTs were actively deployed in several emergencies, including Yemen, Somalia, Afghanistan, and Syria.

Establishing a pool of global MERS experts
In October, 60 high-level public health and MERS practitioners, researchers, and experts met in Abu Dhabi to establish a pool of experts that can be deployed rapidly during any outbreak of the disease.
Since the identification of Middle East respiratory syndrome (MERS) in 2012, over 2200 cases and more than 800 deaths have been reported. More than 90% of these cases were reported from the WHO Eastern Mediterranean Region, making MERS one of the biggest health security threats in the Region and creating the need for additional expertise - a need to which this pool will respond.

Pandemic Influenza Severity Assessments in Afghanistan, Lebanon, Morocco, Egypt, Oman
Understanding the severity and timing of influenza seasons is crucial to plan the right response measures, at the right time, place, and scale. One tool to obtain this understanding is the so-called Pandemic Influenza Severity Assessment, or PISA. A PISA includes three parameters assessing the severity of outbreaks of influenza-like illness (ILI): transmissibility, meaning how quickly the outbreak can spread; seriousness, meaning how deadly the outbreak is; and impact, meaning the pressure on the health system.
In 2018, Afghanistan, Lebanon, Morocco, Egypt and Oman all conducted PISAs, and in November WHO, the Centers for Disease Control and Prevention, and the Global Influenza Programme held a four-day regional PISA workshop in Tunis.

Extensively drug-resistant typhoid fever in Pakistan
In November 2016, Pakistan saw the emergence of a strain of Salmonella Typhi (the bacteria which causes typhoid fever) which is resistant to the most commonly available antibiotics. The outbreak of so-called ‘extensively drug-resistant’ (XDR) typhoid has so far caused 5274 cases and zero deaths.
In response to the outbreak, WHO supported Pakistan’s national and provincial governments with a field investigation mission in November 2018. The mission gathered more information on the extent, size and geographic spread of the outbreak, on the case definition being used to recognize and detect cases, on underlying risk factors contributing to the outbreak, and on the clinical efficacy of drugs being used to treat the disease.

Improving influenza detection and identification capacity
Knowing exactly the strains of influenza which are circulating in any outbreak is key to planning and executing an adequate response. To help countries improve its capacity, WHO in collaboration with its WHO’s Collaborating Centre for Surveillance, Epidemiology and Control of Influenza based in Atlanta (USA) trained influenza experts from 13 countries in November on influenza detection and characterization.
The training focused on all aspects of influenza testing, including testing algorithms to optimize testing efficiency, and real-time reverse transcription polymerase chain reaction (RT-PCR), a standard method to identify influenza strains.

Strategic framework for prevention and control of emerging and re-emerging epidemic diseases discussed and adopted
To guide the work of Member States on infectious hazard management, WHO and its partners discussed and adopted a new strategic framework during a regional meeting held in Jordan in December 2018.
The strategy aims to help countries’ realize the highest possible level of health for all, by eliminating the risk of re-emerging diseases such as rabies, cholera and yellow fever and also guiding timely response efforts to infectious hazards like dengue, Middle East Respiratory Syndrome, chikungunya, extensive drug resistant typhoid fever, and more.
Over the next five years, Member States will take the lead in implementing the framework document, which includes a clear vision and mission, detailed strategic plans, a clear analysis of present and future challenges, and a monitoring and evaluation framework to measure impact over time.








