WHO in Syria
What care looked like in Syria 2025: Key moments in photos
30 December 2025, Syrian Arab Republic – In 2025, Syria’s health system continued to operate under sustained pressure, shaped by years of conflict, displacement, economic strain and recurring emergencies. Working with the Ministry of Health and health partners, WHO focused on protecting access to essential health services during a fragile period of...
Strengthening national capacity to assess and address malnutrition across Syria
Dr Lina Wanli, Nutrition Programme Coordinator at Aleppo Health Directorate, explains the use of the SMART methodology during a national training workshop on malnutrition surveys. Photo credit: WHO 29 December 2025, Aleppo, Syrian Arab Republic – Without reliable data, malnutrition can remain hidden, delaying timely action for people most in...
Standing with Syria through a year of transition
Dr Jaber Al-Omar examines a young patient at Ma’arrat An Nu’man public health centre that was rehabilitated and supported by WHO. Photo credit: WHO 28 December 2025, Damascus, Syrian Arab Republic – When 72-year-old Ali Ibrahim from rural Tartous was told he urgently needed heart surgery, he feared the worst. Private care was far beyond his means...
WHO welcomes NOK 10.2 million from Norway to strengthen Syria’s national health information system
WHO staff during a visit to Ma’arrat An Nu’man Primary Health Centre, where children and families are accessing services following the restoration of the facility. Photo credit: WHO 24 December 2025, Damascus, Syrian Arab Republic –The World Health Organization (WHO) welcomes a NOK 10.2 million contribution from the Government of Norway to...
A father’s commitment strengthens routine immunization in Syria
Abu Tarek’s youngest son sits on the floor of their shelter. Photo credit: WHO 21 December 2025, Idlib, Syrian Arab Republic – In a displacement camp in Afrin, Abu Tarek sits with his youngest son as the morning vaccination round begins. Since arriving at Khazan Camp five years ago, he has made one decision without hesitation: to keep every one of...
National event brings sectors together to address rising antimicrobial resistance in Syria
15 December 2025, Idlib, Syrian Arab Republic – The Ministry of Health, with support from WHO, held a national event in Damascus to strengthen Syria’s response to antimicrobial resistance (AMR) through a One Health approach that brings together the human health, veterinary, agriculture and environmental sectors. More than 100 participants joined...
A grandfather’s quiet routine inspires confidence in vaccination in Syria
Abu Yassin spends time with his grandchildren at their tent in Idlib. Photo credit: WHO 15 December 2025, Idlib, Syrian Arab Republic – In a tent not far from a busy vaccination point in Idlib, nurse Amal moves among parents with the steady assurance of someone who has spent years rebuilding trust in immunization. A mother of four, she begins...
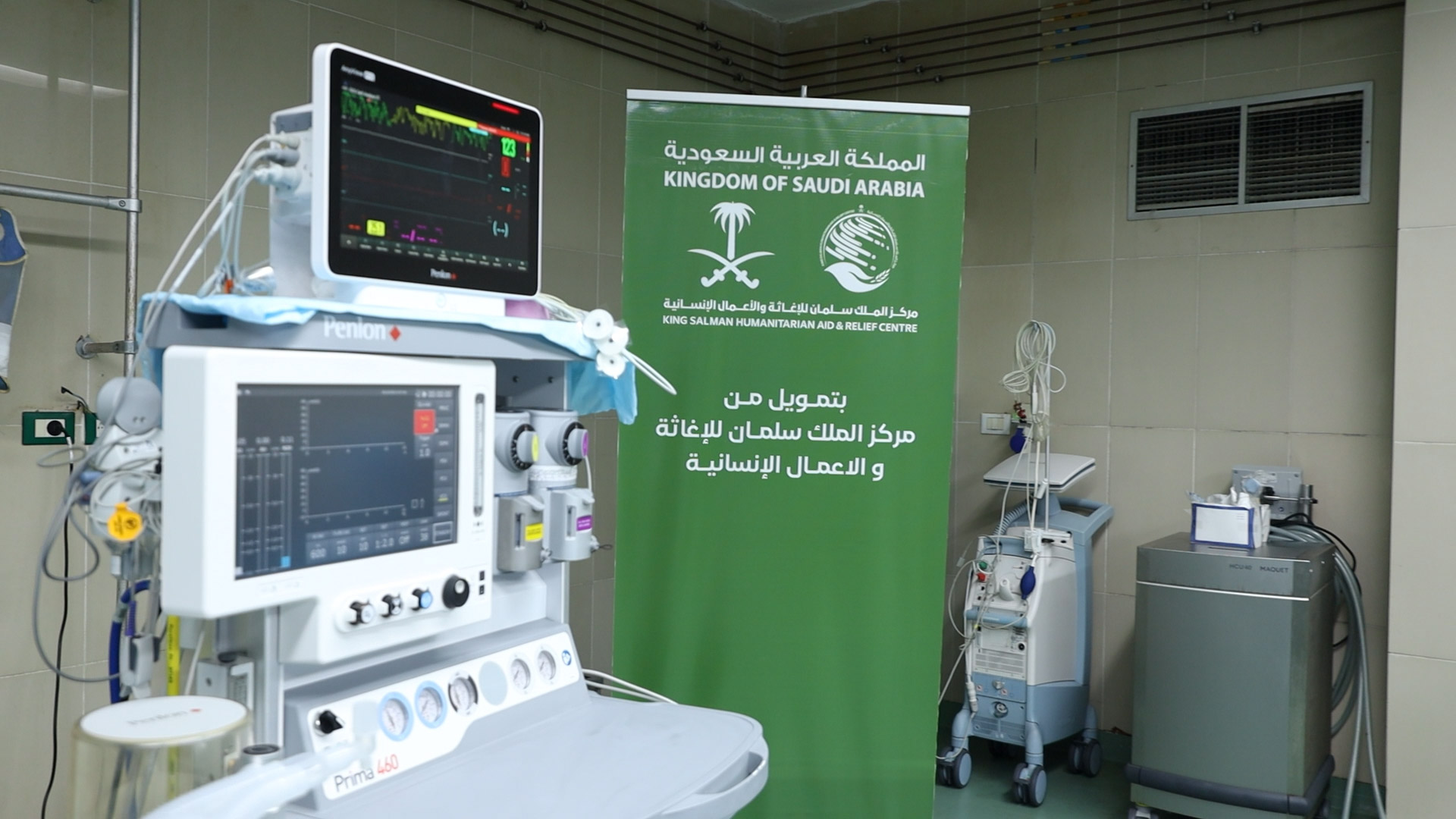
Patients in Tartous see safer surgeries and improved care thanks to new equipment
14 December 2025, Tartous, Syrian Arab Republic – When 72-year-old Ali Ibrahim from rural Tartous was told he urgently needed heart surgery, he feared the worst. Private care was far beyond his means, and travelling long distances was not an option. But at Tartous National Hospital, strengthened with new medical equipment, Ali received the care...
From bedside to classroom, Syrian nurses lead a new chapter in childhood cancer care
11 December 2025, Syrian Arab Republic –In the pediatric oncology ward of Aleppo University Hospital, nurse Nour Al-Huda Al-Yazji moves quietly between beds, checking IV lines, adjusting doses and bending down to catch the shy smiles of children who have learned to trust her. Nurses from Aleppo, Idlib, Lattakia and Damascus who participated in...
WHO and Qatar Charity sign new agreement to strengthen maternal and child health services in Syria
7 December 2025, Damascus, Syrian Arab Republic and Doha, Qatar– The World Health Organization (WHO) and Qatar Charity have signed a US$ 500 000 agreement to expand access to maternal and child health services in Syria, supporting national efforts to sustain lifesaving care and reinforce the resilience of the public health system. The agreement was...