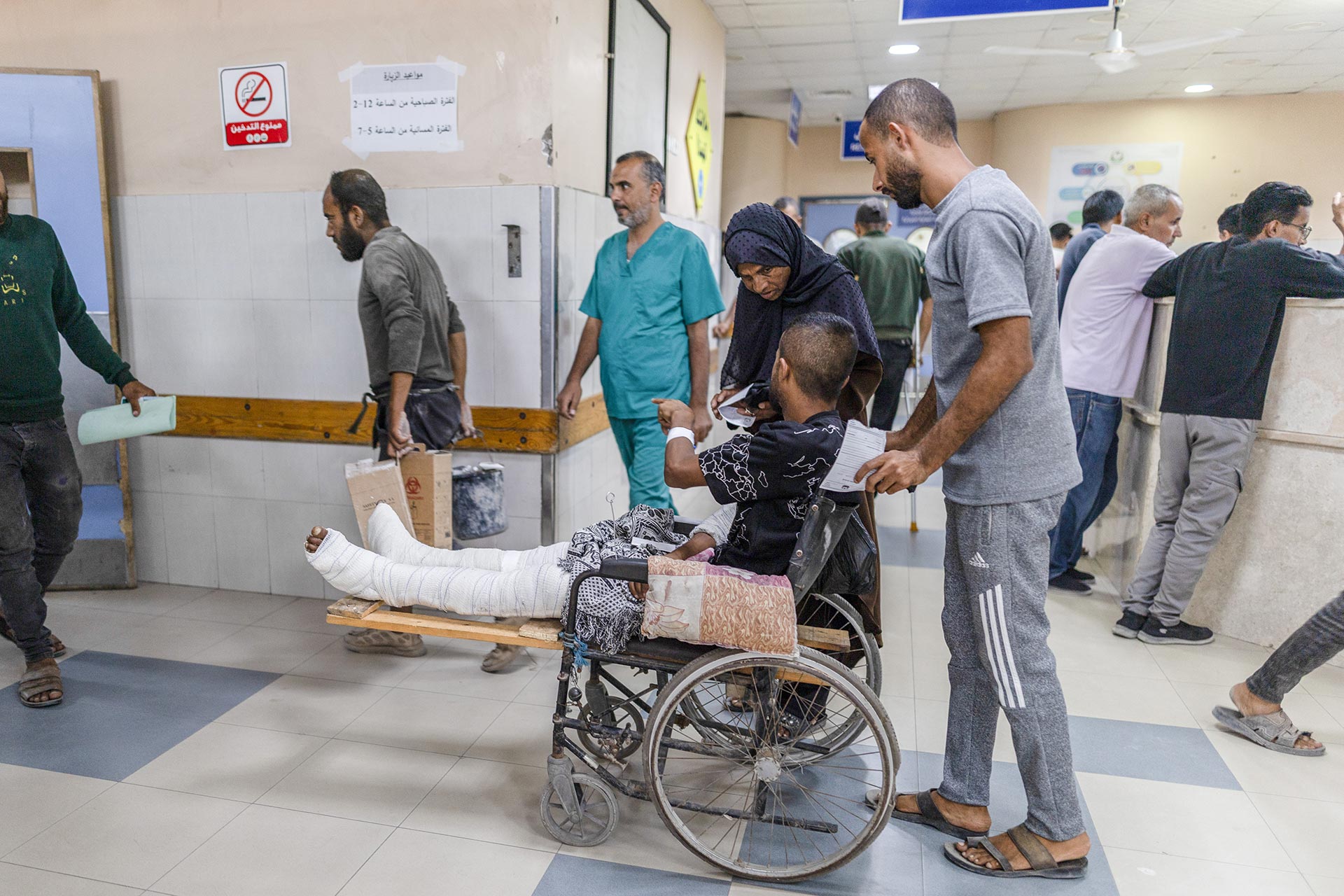
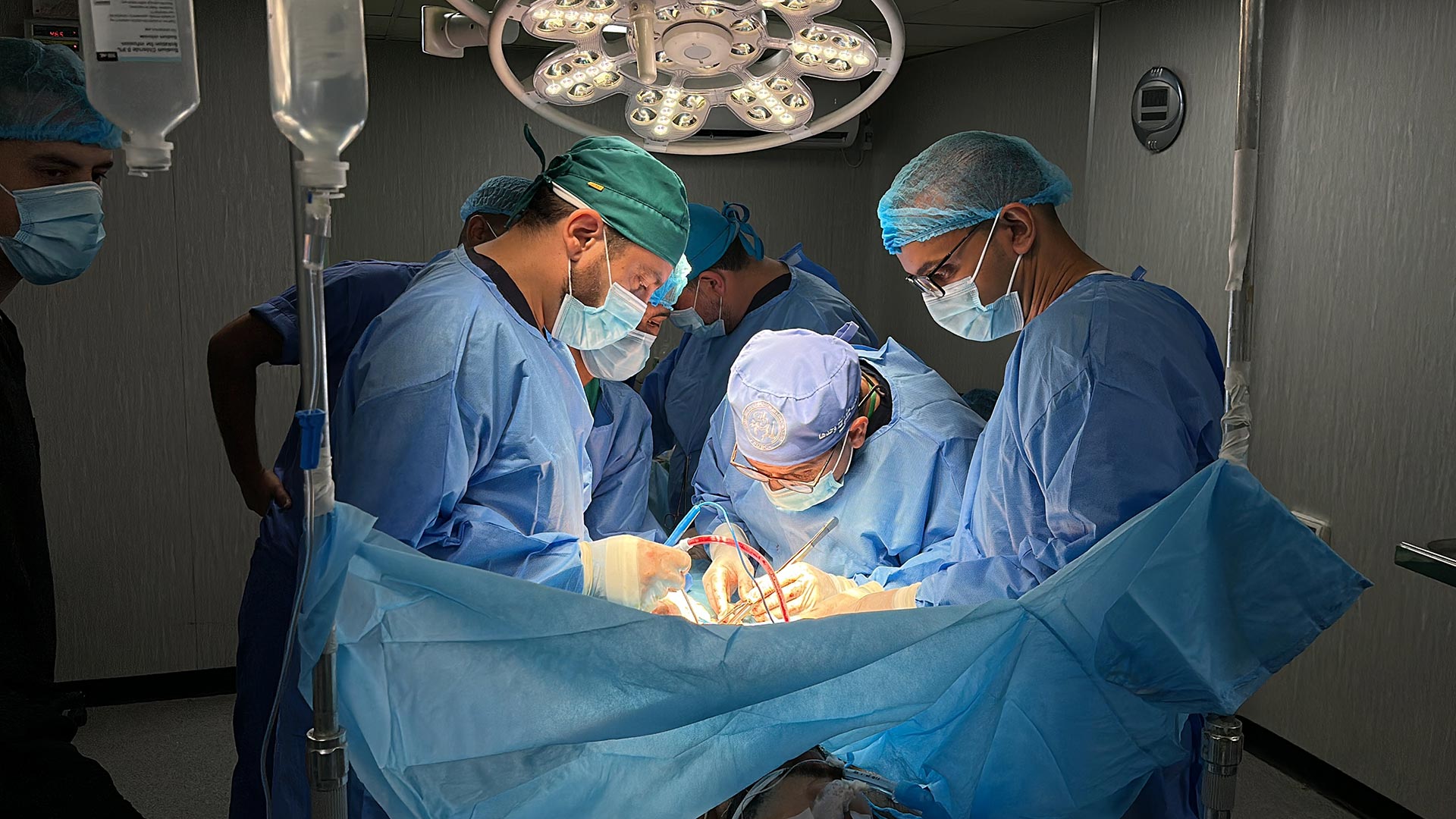
 International EMTs performing a surgery in Public Health Hospital in North Gaza
International EMTs performing a surgery in Public Health Hospital in North Gaza
The scale of death and injury was an overwhelming burden that most health systems anywhere in the world would have not been equipped to bear.
When conflict overwhelmed Gaza's health system, the pressure on trauma care became almost unimaginable. In this episode, three experts who were on the ground speak with WHO: a national emergency medical team leader, a WHO EMT coordinator, and a WHO trauma surgeon. Together, they recount what it took to treat the injured — triaging patients amidst insecurity, transferring them from hospitals that were near active conflict, making impossible decisions in real time, and keeping care going when supplies, staff, and safety were all running out. From the story of one patient moved three times across a collapsing health system, to the role of the national emergency medical team in keeping Shifa Hospital functioning, this episode is human account of resilience to keep health care going.
Guests
Dr Thanos Gargavanis, WHO Regional Trauma Expert, WHO EMRO
Dr Motasem Salah, Team Lead National Emergency Medical Team (EMT) in Gaza, Shifa Hospital
Dr Heba Alnajjar, WHO Emergency Medical Team Coordinator, WHO oPt
Transcript
Egmond Evers (00:05)
Welcome back to the Frontline Shift podcast by WHO that looks at what it really takes to keep healthcare going in Gaza through coordination and deployment of emergency medical teams. I'm your host, Dr Egmond Evers, Health Emergencies Team Lead for WHO in the occupied Palestinian territory (oPt).
Luca Pigozzi (00:21)
And I'm Dr Luca Pigozzi, Acting in Charge of the WHO office in Gaza.
Egmond Evers (00:26)
During over two years of conflict in Gaza, healthcare workers have faced an almost impossible task managing a constant stream of catastrophic traumatic injuries in a healthcare system pushed to its limits.
Luca Pigozzi (00:37)
Since October 2023, nearly 172,000 people have been injured and over 72,000 killed. These figures are almost impossible to comprehend, for a health system already stretched beyond capacity, operating under bombardment and with dwindling supplies. The scale of death and injury was an overwhelming burden that most health systems anywhere in the world would have not been equipped to bear.
Egmond Evers (01:07)
In this episode, we explore how health facilities responded to traumatic injuries under relentless pressure, how care was delivered despite severe shortages of supplies and staff, and what is being done to build resilience and ensure the health system can respond to future emergencies.
This is the Frontline Shift
Luca Pigozzi (01:28)
With us today, we have Dr Motasem Salah, Team Leader of the National Emergency Medical Team (EMT) in Gaza, deployed at Shifa Hospital. The National Emergency Medical Team was founded in 2021 and has been deployed in Shifa Hospital since September 2024 to support the delivery of emergency care. We have also Dr Heba Alnajjar, WHO Emergency Medical Team Coordinator based in Gaza and part of many critical missions that WHO conducted during the conflict to support hospitals and health systems.
Egmond Evers (02:02)
And Dr Thanos Gargavanis, WHO Regional Trauma Expert and Surgeon who was based in Gaza running WHO missions and operations during the peak of the crisis.
Thanos, you were part of the response from the very beginning and carried out some very critical missions. Tell us about what you saw about the scale of the human tragedy and how the health system coped.
Thanos Gargavanis (02:23)
Hello, everyone, and thank you very much for having me. When this dreadful crisis started, the number of casualties and fatalities that we saw were exceeding anything that we had seen before. The health system in Gaza was already in a difficult situation before this crisis. The World Health Organization had been investing for quite some time to establish an effective trauma system in Gaza. And the results were that we had established a sustainable trauma pathway, meaning that there was a way to make sure that every trauma patient from the point of injury to rehabilitation would be following a precise pathway, meaning that there was somebody that would be taking care of him in the first phase that was pre-hospital care. They would be taken either to a trauma stabilization point or to initially primary health care center for the initial stabilization. And then based on the severity of the injuries, he or she would be referred to a designated hospital or not.
All this work was of extreme importance when this crisis started, because there was an institutional memory and the systematic capacity made everything easier, not easy, easier to respond. During the first moments of all this crisis, when we first set foot on the ground, the images that we have seen inside the hospitals and inside the improvised receiving facilities were really devastating. We have seen people lying on the floor with blood gushing out of open, devastating injuries. We have seen extremely overwhelmed and heroic medical personnel and nursing personnel who were trying to do their very best with the limitation of resources available. We have seen families bringing their beloved ones mourning for the death and for the loss of others that they could not save on time. And we have seen a system that was trying to reinvent itself while the disaster was ongoing.
Luca Pigozzi (04:48)
Thank you, Thanos. What you just described is truly devastating.
Egmond Evers (04:52)
As of January 2026, there have been more than 3400 serious injuries to the head, neck and spine. Over 22000 limb injuries. More than 5000 amputations, over 3000 burns and over 8500 other major injuries. Each one of those numbers is a person. A life changed forever.
Luca Pigozzi (05:15)
Thanos, back to you. You were on the ground helping to get medical supplies to hospitals and transferring patients from one facility to another for the safety or appropriate care. Throughout the conflict, are there any particular cases that you remember and you want to share with us?
Thanos Gargavanis (05:35)
Each and every case has its own story, and I wouldn't like to be unjust to others. However, the case that always comes to my mind and the effort that the World Health Organization, along with partners and the existing health system, invested to make sure that we save lives — brings me to a patient of around 40 years old. A man that we had to move three times as the front of the conflict was changing.
The man had sustained devastating spinal column injuries in November 2023 in Gaza City. He was moved to a nearby hospital, Al-Ahli Hospital, where unfortunately there was not enough equipment and supplies for a proper neurosurgical stabilization of the spinal column, and the patient was waiting for a referral to a safer haven and to another facility where he could be operated. That was the first time that he joined one of the WHO missions in November 2023, when we moved him, and took him from Al-Ahli Hospital to European Gaza Hospital.
From European Gaza Hospital before Christmas, the patient had to move again and went to Nasser Medical Complex because, again, there was extreme lacking of supplies and equipment and the surgical personnel could not deliver what in other circumstances could should be delivered. Finally, the third time that we have seen the same patient was in February 2024, when the front was moving that fast that Nasser Medical Complex got engulfed in the conflict. Then, in a series of four consecutive missions, the World Health Organization, along with PRCS and other UN agencies, we relocated the last remaining 87 patients that were remaining in the hospital.
It still strikes me that one of these patients was this man. The man that had initiated his treatment, travelling from Al-Ahli Hospital in Gaza City, then to European Gaza Hospital and then ended up again in Nasser Medical Complex. And unfortunately, he was never able to be properly treated and properly operated because we were never able to source the necessary equipment and supplies that were needed for the stabilization of his fracture.
Finally, the patient ended up in one of the field hospitals where another suboptimal solution was chosen. He was treated in a more conservative way and with a different surgical technique to stabilize the spinal column. However, what relieves me is the fact that the man has remained able to move his legs and toes, because what we were afraid was that eventually he would be paralyzed from the waist and below for life. And it still strikes me that none of his kith and kin were able to be with him during all this trouble.
Luca Pigozzi (09:13)
Thanos, what you have described is, sadly, I'm sure, the story of countless patients injured during this conflict, people forced to move from place to place and unable to access the care they needed.
Egmond Evers (09:26)
Heba, like Thanos, you've been right in the thick of it in Gaza. You've been doing critical missions, triaging patients, and making decisions about patient referrals. Can you take us through the process a little? What did it look like on the ground, and what were some of the most difficult calls you had to make?
Heba Al-Najjar (09:43)
Thanks for having me on today's episode. I want to talk about something that defined much of our work during the crisis in Gaza, actually moving patients out of the hospitals that were no longer safe or functional, some facilities had been attacked. Others were located in areas under active evacuation orders or close to hostilities. Our role was not only just coordination. We were on the ground transferring critically ill patients and facilitating where they could continue receiving care. Let me share some of what that looked like during this time. One patient we transferred had burns covering 70% of her body. She had no family with her, no companions at all. We moved her in an ICU ambulance, but at the checkpoint, we were held for a significant wait. As medical team, we were carefully managing her sedation, keeping her stable and keeping her out of pain until we could get her to another ICU and hand her over to another medical team. The hospital had also become shelter. Entire families were living inside the buildings and in the surrounding areas, all of them were under evacuation orders. Many had no place elsewhere to go. When we arrived at the hospitals, many of the families were approaching us asking us if we can move them as well with no other way out. It was a truly desperate situation. Some transfers required a lot of real time decisions. Required a lot of medical care during the time of transferring to patients, I remember one case with CADUS. The convoy was ready to move patients loaded, and all of a sudden one of the staff member came to us. This staff member was telling me that the patient had just started to be desaturated, and had a chest tube with him, and then it was a decision, shall we just leave him in an empty hospital, or we take the decision and we accept the risk and just move him with us? We made the call to take him with us, and if he got deteriorated during the transportation in the road, we would stop the convoy, stabilize him, and move again. This was one of the most difficult decisions we took in the field. And then there were a lot of hospitals like themselves. Those hospitals was not able to receive patients as there is no clinical stuff remaining inside those hospitals. We would arrive and find patients scattered all over inside the hospital, in different wards, different floors. We didn't have any staff member who can hand over the patients to us, no documentation, and sometimes very, very little paperwork with the patient. We had to go through the building, looking for the patients, trying to find out where they are sitting, and assess them, stabilize where needed, and then put them together and try to collect them and put them inside the ambulances and find out whatever paperwork would be available with them and can help, because when we arrive to the other hospital, when they should be receiving the patient they need, something to work with and to start, at least to know what this patient had in the other facility before. Actually, none of it was easy at all. We were not only dealing with injuries that very complicated and very complex from all kinds, but also many hurdles delaying and getting patients the healthcare that they needed.
Luca Pigozzi (13:20)
Thank you so much, Heba. What has the role of the emergency medical teams been in providing surge capacity and building resilience of the health system during the emergency response in Gaza?
Heba Al-Najjar (13:32)
Since the EMT program was officially activated in December 2023 emergency medical teams have become an essential part of the healthcare system in Gaza, working shoulder to shoulder with the local healthcare workers and trying to keep it functional under extraordinary pressure. The numbers speak to the scale of the effort that the EMTs conducted, starting from December till now, more than 44 partners and organizations deployed EMTs regularly, more than 56 teams deployed, and more than 4 million consultation were achieved since the start of the crisis. But the numbers only are telling part of the story. It's not telling everything. Many Palestinian health care workers couldn't reach even their facilities and where they are working, they were displaced. Some of them were killed and some forced to leave the country, searching for the safety of their families and for their children. EMT stepped into this gap and tried to support as much as possible, but it was never about replacement. It was all the time about how we can work together to support the healthcare system. It was always about integration and partnership. They were also not only surging and trying to provide services, but also tried to train the local staff member, transferring the skills to them and trying to build their capacity, including inside emergency departments, inside the operation theater, everywhere, where they were working together in the most difficult conditions, even during mass casualties, they were trying to make them aware how to deal with the situations in a proper manner. Actually, what helped us to have a successful response during the last period was the strong coordination framework behind that between all of the EMTs, Minister of Health, local partners and other international NGOs, different organizations deployed and were working together inside. All of them were sharing a same goal, which is ensuring that patients have access and receiving quality of care, and all of them were trying to ensure the minimum standard, regardless all of the circumstances we were working under. One of the most important lessons learned during the crisis here inside Gaza, it's about the critical importance of building national capacity. There were times when international teams and organizations couldn't get in and didn't have access. Some specialized teams were denied access completely. The reality that we understood while we are working that we need to focus on building national EMTs, and actually we succeeded in building two national EMTs during the last period. Teams can completely deploy by themselves, sustain longer and operate independently under whatever circumstances, under all of the risks. When international support maybe can be delayed or blocked so nationals can take the lead and working and supporting their healthcare system. Currently, in those days, international EMTs are playing a mentorship role. They are trying to equip and train all of the national emergency medical teams with all of the tools and all of the equipment, and providing all of the technical guidance for them, and trying to hold the line on their own until additional so the national EMT can hold the line by their own and try to provide the needed services until additional support can come and arrive.
Egmond Evers (16:58)
Thanks, Heba. Dr Mutasem, could you tell us a bit about how the national EMTs have been helping to manage the emergency caseload at Shifa Hospital?
Motasem Salah (17:08)
In April 2024, Shifa Medical Complex, the largest tertiary health care facility in Gaza Strip, was heavily damaged and effectively put out of service during the war. The hospital was left unable to function as a medical facility. Most buildings and equipment were destroyed. Complete destruction of all operation systems and the hospital could no longer operate normally as a hospital.
In response, Ministry of Health worked in rehabilitating the outpatient clinic building to serve as an emergency department. In 2024, through the EMT and with the support of MoH and WHO, Shifa Medical Complex was reopened with the capacity of thirty beds, two operation rooms, intensive care unit beds, and laboratory services, and severe cases needing admission were referred to other hospitals.
A national EMT played a vital role in managing emergency and trauma caseload. The medical team at Shifa Hospital implemented an effective triage system to control the flow of patients. Triage was conducted outside the emergency department to manage the cases efficiently.
The EMT improved the emergency response capacity with support of WHO. We trained all the staff in primary health care and in emergency departments.
Luca Pigozzi (18:42)
Thank you very much, Dr Mutasem. In fact, the dedication of the national EMT in Gaza is priceless, and the restoration of emergency care at Shifa Hospital was just due to the deployment of the national EMT. So again, big thanks to you and to the national team.
Thanos, let's get back to you. As the work on rehabilitation and recovery of Gaza proceeds, what are the key needs and challenges in ensuring a resilient health system that can cope with an influx of casualties?
Thanos Gargavanis (19:15)
What everybody needs to understand here is that the World Health Organization stepped in to address the needs that came out of this conflict, because it was really the last resort. The World Health Organization stepped in to provide supplies, to provide medication, to support and coordinate international emergency medical teams, mentor, and do the very best so that the national emergency medical team delivers at the best of their capacity and eventually try to address different gaps at different levels of care.
However, we are far from over right now. The system is struggling to get back to where it was. And I hope that with the steady flow of supplies and medical equipment and surgical equipment, we will never see again cases that ended up getting amputated because of the inability of the entire health system to save the limb. When we're talking of saving a limb, we all have to understand that this is not something that can be attributed to just one action. You must be having adequate care in the first step when you receive the patient so that you decrease the possibility of future infections. You must be having adequate nursing capacity. You must be having enough food so that the patient is properly nourished and is able to respond to the needs of his healing process. You must be having operation theatres that are clean and can be used to manage very complex injuries without exposing further the patient to danger.
Unfortunately, during the peak of this war, we have seen numerous times that patients had to be subjected to amputations because the system was not able to provide all the necessary means to save these limbs. I truly hope that with a joint effort from the international community, other health partners and the World Health Organization, the system will be able to sustain the reconstruction — that it's a long process, a process that requires commitment not only from the health system but from the community as well, so that the patient that goes through this process gets supported all along the way. And eventually we will be having people that, after their injuries, will be able to return to their community as equal members that are able to go outside, support their families, work, and have a life that resembles normal life as much as possible.
More investment is needed. More commitment is needed. Open passages are needed and a sustainable medical evacuation for those that cannot be treated inside Gaza is also needed.
Egmond Evers (22:30)
Thanks a lot, Thanos. As you've mentioned, Gaza will really need continued support to be able to transition to recovery and reconstruction. What we've heard today is a testament to the courage of health workers who would not stop, of patients who didn't give up, and of a health system that, despite everything, refused to collapse.
Luca Pigozzi (22:49)
The road to recovery in Gaza is long and the needs are immense. But as today's conversation makes clear, the commitment to rebuild and to do so in a way that prepares for the future remains as strong as ever.
Egmond Evers (23:03)
To everyone working on the front lines of this crisis, inside hospitals, in the field and behind the scenes, thank you. This has been the Frontline Shift. These are your hosts, Egmond and Luca, signing off.