Episode 5: Malnutrition in Gaza
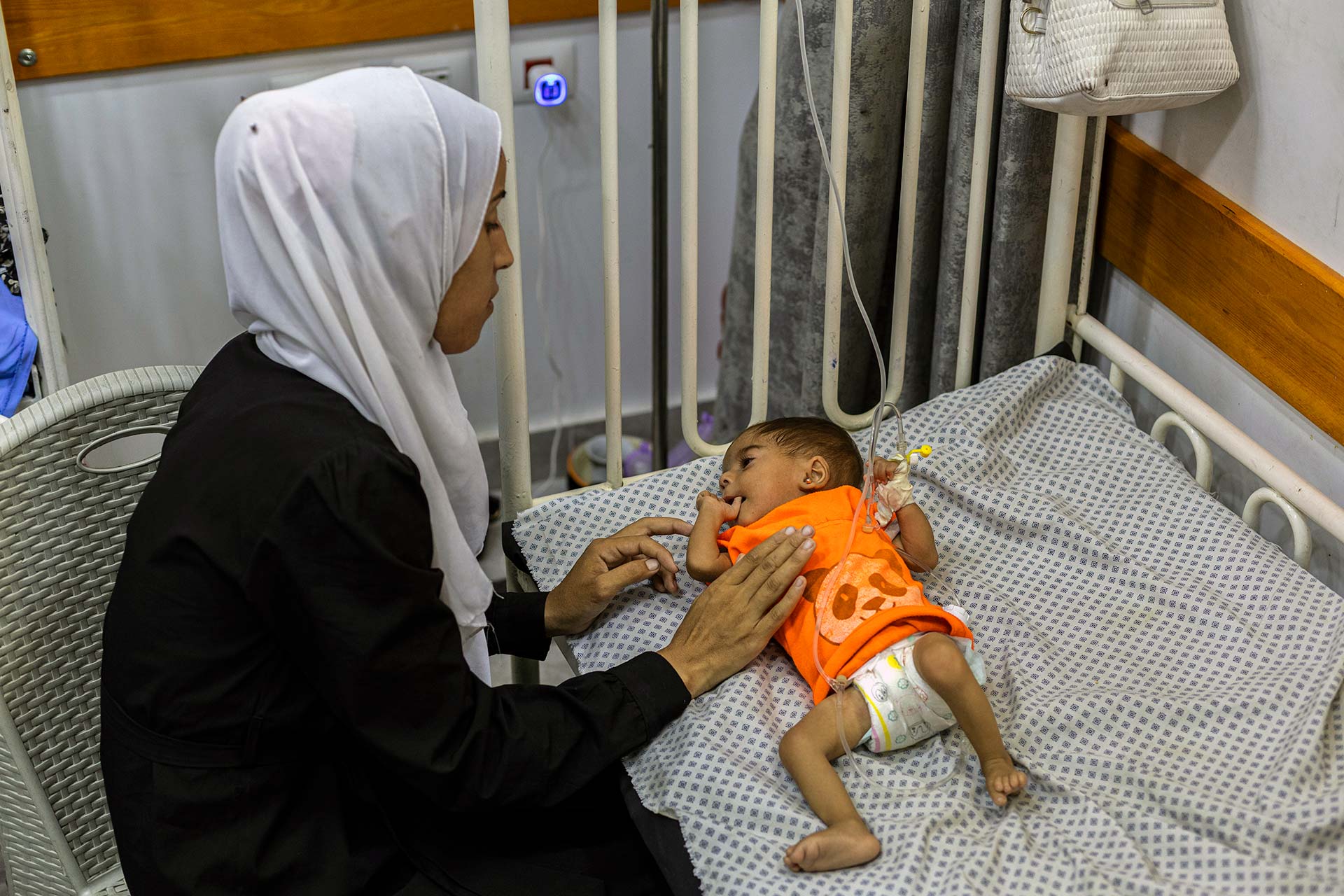 A child with severe acute malnutrition (SAM) admitted to the inpatient SAM stabilization unit at Patient Friends Association Hospital. Photo credit: WHO
A child with severe acute malnutrition (SAM) admitted to the inpatient SAM stabilization unit at Patient Friends Association Hospital. Photo credit: WHO
The malnutrition crisis in Gaza reached unmatched scale — at its peak, the entire population of approximately 2.2 million people faced acute food insecurity.
Before the conflict, malnutrition in Gaza was rare. By 2025, it had become one of the key health issues of the conflict. In this episode, Dr Dalia AbuJahel, WHO's Reproductive Health Officer, and Salwa Al-Tibi, Country Representative for emergency medical team Med-Global, discuss the scale of the malnutrition crisis in Gaza, how it unfolded, and what the response has looked like on the ground.
They speak to the human cost — including the story of two sisters, Jana and Joury, who died from severe acute malnutrition despite receiving care — and reflect on the broader impact on paediatric and maternal health, from rising rates of prematurity and low birth weight to overwhelmed neonatal units and shortages of essential supplies. They also look at what recovery will require, and why the situation, while stabilising, remains fragile.
Guests
Salwa Al-Tibi, Country Representative, Med-Global
Dalia AbuJahel, Reproductive Health Officer, WHO oPt
Transcript
Egmond Evers 00:05
Welcome back to The Frontline Shift, a podcast by WHO that looks at what it really takes to keep healthcare going in Gaza through coordination and deployment of emergency medical teams. I'm your host, Dr Egmond Evers Health Emergencies Team Lead for WHO in the occupied Palestinian territory.
Luca Pigozzi 00:21
And I'm Dr Luca Pigozzi, Acting in Charge of the WHO office in Gaza.
Egmond Evers 0:27
Children have paid a devastating price in the two years of conflict in Gaza, and we're not just talking about violence, displacement, disease and hunger have been equally devastating and often deadly.
Luca Pigozzi 0:37
In today's episode, we focus on how the conflict, restriction of aid and famine escalated malnutrition and also impacted the overall paediatric care in Gaza and the role of the emergency medical teams in supporting this.
Egmond Evers 0:51
We will also focus on the immense challenges of delivering healthcare for children during the conflict and what is needed to meet ongoing needs.
This is The Frontline Shift
Luca Pigozzi 1:03
With us today we have Salwa Al-Tibi speaking to us from Gaza. She's the Country Representative from Med-Global. Med-Global is an emergency medical team working in Gaza and deploying international teams since January 2024. We also have with us Dalia AbuJahel. She's the WHO reproductive health officer who was born and raised in Gaza.
Salwa Al-Tibi 1:27
Hello. Thank you so much for the invitation.
Dalia AbuJahel 1:31
Hello and thank you for the invitation.
Egmond Evers 1:34
Aid restriction has been a significant and persistent challenge in the conflict in Gaza, a complete blockade on the entry of all humanitarian aid, including food, medicines and other essential supplies, lasted between early March and mid May 2025. Just under three months. The restriction on entry of aid at scale has remained an issue throughout the conflict, although the availability of food in Gaza has improved since the ceasefire in October 2025.
Luca Pigozzi 1:59
One of the most alarming consequences of these aid restrictions in Gaza was the dramatic rise in malnutrition. Before the conflict, Gaza had enough food to feed its population, and malnutrition was really rare.
Egmond Evers 2:13
At that time, 0.8% of children under five years of age were acutely malnourished. But by February 2025 according to the United Nations IPC report, the figure was between 12 and 16% in the north of Gaza. In that area, the shortage of food was most severe given access restrictions for humanitarian staff and due to the intensity of ground operations.
Luca Pigozzi 2:35
Just to explain to our listeners, the IPC is a joint partnership of 21 organizations, including also us, including also WHO, who work together to determine the severity and extent of acute and chronic food insecurity and acute malnutrition situations according to internationally recognized standards.
Egmond Evers 2:54
It's no surprise that restriction on the entry of food eventually led to famine in parts of Gaza in late August 2025 one of the darkest chapters of this conflict. Butthe malnutrition situation was already dire much earlier in the year, even before famine was formally declared in parts of Gaza. Despite famine conditions ending by December, the damage had already been devastating, compounded by the destruction of the healthcare system.
Luca Pigozzi 3:19
Children and also adults died from the combined effects of malnutrition and diseases. Malnutrition weakened their bodies, making it harder to heal from injuries and fight off common communicable diseases like diarrhea and respiratory infections.
Egmond Evers 3:37
In turn, these infections increased the body's requirement for nutrition while reducing nutrient absorption, resulting in worsening malnutrition. With healthcare out of reach and access to clean water and sanitation severely limited illness and death increased.
Luca Pigozzi 3:53
Dalia, what has been the scale of the malnutrition crisis, and what is the situation as of now? How been the response delivered?
Dalia AbuJahel 4:02
As you mentioned, Luca, malnutrition was never reported in Gaza. The malnutrition crisis in Gaza has reached unmatched scale over the past years, particularly in 2025 when conditions in parts of the Gaza Strip, deteriorated into famine. So at its peak, and according to the IPC analysis, the entire population of approximately 2.2 million people living in Gaza faced acute food insecurity, with around 470,000 people in catastrophic hunger, IPC Phase Five, definitely, children have been disproportionately affected, with an estimated 71,000 children required the treatment from acute malnutrition, including around 14,000 children treated for severe acute malnutrition (SAM), and more than 1000 children were treated at SAM stabilization centers for severe acute malnutrition with complication, which is a life threatening condition with high morbidity and mortality. In some areas, acute malnutrition rates surged dramatically, with reports of up to one in five children affected from malnutrition, especially in Gaza Governorate, where famine was declared in August 2025. Malnutrition related deaths have also been reported in 2025, particularly among younger children. And the total number that has been verified by WHO, Minister of Health and Nutrition Cluster reached 421 of which 113 were children. Definitely, the crisis has been driven, as you mentioned, by the collapse of the food system, the severe restriction on the entry of humanitarian aid, the widespread displacement, destruction of the health services and poor WASH infrastructure, with lack of access of safe water as well as adequate nutrition. As of early 2026 the situation remains extremely serious, although the famine condition have been pushed back following relatively increased humanitarian access. However, according to the latest IPC analysis, an estimated 1.6 million people are expected to be facing high levels of acute food insecurity through mid April 2026, this includes approximately 101,000 children less than five years who are projected to be requiring treatment from malnutrition. Other vulnerable groups have emerged, including around 36,750 pregnant lactating women, 25,000 infants below six months, as well as 120,000 children aged 5 to 17 years. So while the immediate risk of famine have been reduced, still Gaza continues to face a larger scale, and we can say protracted malnutrition crisis, and a situation that will remain fragile unless there is a sustained humanitarian support that is secured. WHO worked in collaboration with the Minister of Health, Health Cluster and the Nutrition Cluster to respond to the malnutrition crisis in Gaza Strip, WHO focused on establishing severe acute malnutrition stabilization centers, which are centers that are dedicated for the inpatient treatment of severe acute malnutrition with complication. Since the start of the conflict, WHO supported the establishment of severe acute malnutrition stabilization centers all over the Gaza Strip. Ten stabilization centers were established in different governorates of Gaza Strip, out of which seven are remaining operational until now. The main challenge for establishing the stabilization center in Gaza was the lack of availability of enough space for integration of stabilization services in the inpatient facilities.
Egmond Evers 7:30
Dalia raises an important point, even as food access improved following the ceasefire and famine conditions were reduced in December 2025 a large number of people in Gaza are still expected to face acute food insecurity. This is because following the ceasefire, while markets improved with better flow of food deliveries, vulnerable families especially are unable to afford food. Nutrient rich foods, particularly proteins, remain scarce and expensive, and this is the reality for many people.
Luca Pigozzi 8:00
There have been so many devastating cases of lives lost due to hunger, something that was entirely preventable and manmade. Dalia, you have been working with the Ministry of Health to verify these cases. Are there any particular ones that come to mind?
Dalia Abu Jahel 8:17
As I mentioned, more than 113 children died from acute malnutrition, but there are two cases, actually they are two sisters, Jana and Joury, who tragically died from the severe acute malnutrition despite receiving care at the stabilization centers. Both sisters were admitted to the stabilization centers multiple times suffering from severe acute malnutrition, with complications mainly fever, diarrhoea, poor appetite, anaemia, dehydration and electrolyte imbalance. Despite each time they were admitted and received care at stabilization centers, they initially in the start showed improvement of their medical as well as a nutritional condition, but the recurrent admission to the SAM stabilization center and the fragility of their condition, and as you mentioned, the poor immunity that is attributed to the malnutrition situation, ultimately led to their death. Joury died first. She was only one and a half years suffering from the severe acute malnutrition with complication. Despite, as I mentioned, receiving the nutritional rehabilitation at two SAM stabilization centers, then Jana, after that, she died. Both of them were admitted more than three times to severe acute malnutrition stabilization centers and received adequate treatment. Both Jana and Joury were supposed to be receiving medevac and to be treated outside Gaza, but unfortunately, both of them died even before having the access for more advanced treatment outside Gaza.
Luca Pigozzi 9:45
Thank you. Dalia, very sad stories. Salwa, your team has been working on treating children with malnutrition. How young have the patients been? What is the caseload like now, and when did you start seeing a reduction in cases?
Salwa Al-Tibi 10:00
In the beginning, we were targeting from zero to five years old, but now we are targeting according to the needs. We are targeting the children from zero to 12 years old. And let me explain so far, the number of the children, is reduced. But last month, for example, at hospital, we received 25 cases with SAM with complications, and 11 of these children were below six months. And it's related to the mothers, because the mother, when she was pregnant, she was, you know, facing a malnutrition. What we are doing inside the stabilization center upon receiving the child and his or her caregiver at the hospital, the measurement are taking, including (MUAC) Mid-Upper Arm Circumference, weight and height based on the child health condition. If severe acute malnutrition is detected, the child will be transferred immediately to the inpatient department to begin the intensive treatment phase. In the same time, we are not working only with the children. We are supporting the caregivers. You know, we work closely with the mothers and caregivers by providing infant and younger child feeding, as I mentioned, awareness sessions to strengthening in nutrition practices and ensure sustainable improvement in the child health.
Luca Pigozzi 11:39
Thank you very much. Salwa, for your testimony. Dalia, could you tell us what are the long term impacts on children's health as a result of malnutrition?
Dalia Abu Jahel 11:50
Actually, the malnutrition situation in Gaza has moved from just not only being an acute emergency, but also is now evolving into a protracted crisis, and definitely it will have long term application for the affected populations, especially the children stunting and developmental delays due to prolonged malnutrition during the critical growth periods. The first 1000 days of any child's life is a very critical growth period which will be likely having an impact on the physical growth as well as the cognitive development, especially girls and adolescents who are facing high risk during the future pregnancies from poorer nutrition as well as health outcomes. Additionally, there will be likely long-term impact on the non communicable diseases risks, especially early life malnutrition increases the susceptibility for metabolic disorders, cardiovascular diseases and other non communicable diseases. Those children are under a very highly stressful condition which will be also affecting their mental health as well as psychosocial well-being, mentioning that the profound destruction, as well as the poor living condition, which will be like having very long term impact on the situation of those children, this actually raises and highlights the urgent needs for not only immediate lifesaving intervention, but as well as sustained investment in nutrition as well as, of course, health system recovery in order to prevent this last public health consequences on the children as well as the future generations.
Luca Pigozzi 13:22
Apart from malnutrition, overall paediatrics and maternal health care has suffered immensely in Gaza. Dalia, what have been some of the setbacks and what is being done to support in expanding services?
Dalia AbuJahel 13:36
Thank you, Luca, as Salwa mentioned, the fact that many admissions involve very young children, underscores that there's a very heightened vulnerability. Among these key challenges is the damage and the closure of health facilities, which has reduced the availability of essential services such as antenatal care service delivery, natal intensive care as well as paediatric treatment, which led to very high challenges in even establishing the stabilization centers, as I mentioned earlier. Additionally, there have been severe shortages of medicines, equipment supplies, which affected not only the quality but also the continuity of the care the healthcare workforce themselves, being Gazan suffering from the same hard living condition. They have been very heavily impacted, being displaced, overworked or unable to even to safely reach their workplaces, additionally, access barrier, including insecurity, transportation concern, population displacement, which have delayed care seeking, often resulting in more severe conditions even at the presentation. To address these setbacks, a lot of efforts are ongoing to restore and expand essential services, including supporting the rehabilitation and functionality of key health services, particularly maternity wards and neonatal units and paediatric departments. There also has been a large focus on larger scale provision of essential medicine equipment as well as supplies, additionally training of healthcare workers and supporting them in order to strengthen the service delivery. In parallel partners are working on expanding the service coverage, especially in areas where access has been better secured, and scaling up the stabilization centers for severe acute malnutrition, and strengthening the primary health care services and improving referral systems in order to ensure the continuity of care. There's also a continued emphasis on coordination as well as health system support to align intervention and prioritize the most affected areas. So a lot of important steps are being taken to expand services and sustained access to resources, as well as long-term investment are still needed and critical in order to fully restore and strengthen the paediatric and maternity healthcare in Gaza Strip.
Egmond Evers 15:45
Salwa, are there enough supplies coming into Gaza to support the care that's needed?
Salwa Al-Tibi 15:50
Still there is a gap. There is, you know, a shortage of medical supplies and disposables and equipment and other also, or let me call the spare parts for some of the equipment. There is a lot of the changes, also, that sometimes we face problems due to the closure of the crossings.
Luca Pigozzi 16:12
Thank you very much Salwa.
Egmond Evers 16:15
Dalia, what are some of the more common pediatric cases that we're seeing now in Gaza?
Dalia Abu Jahel 16:19
We are seeing a very high surge in prematurity in Gaza now. The increase rates of prematurity is reaching 11% of the live births now in Gaza, who are increasingly requiring admission to neonatal intensive care units for a long period, until they are recovering and able to be going with their mothers to the community. Additionally, low birth weight, which is attributed to the malnutrition during the pregnancy, is also surged high in some governorates during the famine crisis. It reached more than 15% of the live birth who are additionally requiring admission to the neonatal intensive care unit, as well as recurrent admission to the paediatric services later on. Additionally, congenital anomalies are being recorded among the newborns now in Gaza, which is also multifactorial, not all, related to only the malnutrition situation, but also to other genetic as well as predisposition, and later on, a lot of studies will be required to to investigate the causes of congenital anomalies. Additionally, children with inborn error of metabolism and metabolic disorders are increasingly requiring admission to the paediatric services. Those children in the past used to be referred outside Gaza for diagnosis of their condition as well as for specialized treatment. Now, they are recurrent admission, recurrently admitted to the pediatric services, as well as to the stabilization center, and unfortunately, they have high morbidity and mortality consequences of their condition with poor availability of the specific treatment now in the Gaza Strip. Additionally, as you know, the high rates of of communicable diseases and the outbreak of communicable diseases is also causing increasing admission of complication attributed to these communicable diseases, acute respiratory tract infection, acute diarrheal disorders, as well as bloody diarrhea, they are increasingly admitted to the paediatric services as leading to more than 100% occupancy rate and in the paediatric hospitals who are barely functioning with limited bed capacity, as well as limited staff working in these hospitals.
Luca Pigozzi 18:43
Dalia, what is needed to improve the paediatric and maternal health care services in Gaza?
Dalia Abu Jahel 18:48
Actually, everything is needed to improve the paediatric and maternal health care services in Gaza, but some of the several critical priorities that are needed to be addressed is: first and foremost, is sustained and unhindered humanitarian access. Without reliable access, it will not be possible to ensure continuity of essential services, timely referrals, or the consistent delivery of care for women and the children. WHO is working tirelessly on securing the entry of supplies as well as medication and equipment in Gaza. Second, there is a need for large scale provision of medicine and supplies and equipment. This includes everything from essential drugs consumable to neonatal and obstetric equipment required for safe deliveries in newborn care and paediatric treatment. Third and the most important, is rebuilding and strengthening the health care workforce, not only addressing shortages, but also supporting the training and retaining the skilled health worker who have been operating under extreme pressure. WHO, throughout the past year and this year, is trying to work on a package of sexual reproductive, maternal, newborn and child healthcare capacity building topics, in order to improve the quality of the healthcare provided to the paediatric as well as to the maternity cases admitted to the hospitals, as well as at primary health care level. Finally, there must be a long term investment in the health system in Gaza, restoring and rehabilitating the healthcare facilities and strengthening the primary healthcare and ensuring the integration of maternity, newborn and child health services. Much more focus needs to be for restoring these services in order to ensure that we have timely as well as availability of services for these vulnerable groups in the Gaza Strip.
Egmond Evers 20:32
The stories we've heard today of children like Jana and Joury and of health workers treating children under impossible conditions, these are not just numbers, not just statistics, they're the lived reality of an entire generation.
Luca Pigozzi 20:46
Access to health services, medical supplies and a sustained commitment to rebuilding, this is what Gaza needs now. Thank you Salwa. Thank you Dalia, for your time and hard work dedication in this emergency response.
Egmond Evers 21:00
And to every health worker and humanitarian who has refused to give up on Gaza, thank you. This has been The Frontline Shift. These are your hosts, Luca and Egmond, signing off.
 A child suffering from malnutrition sets in a tent with his mother. Photo credit: WHO
A child suffering from malnutrition sets in a tent with his mother. Photo credit: WHO
Episode 4: Trauma Care During the Conflict
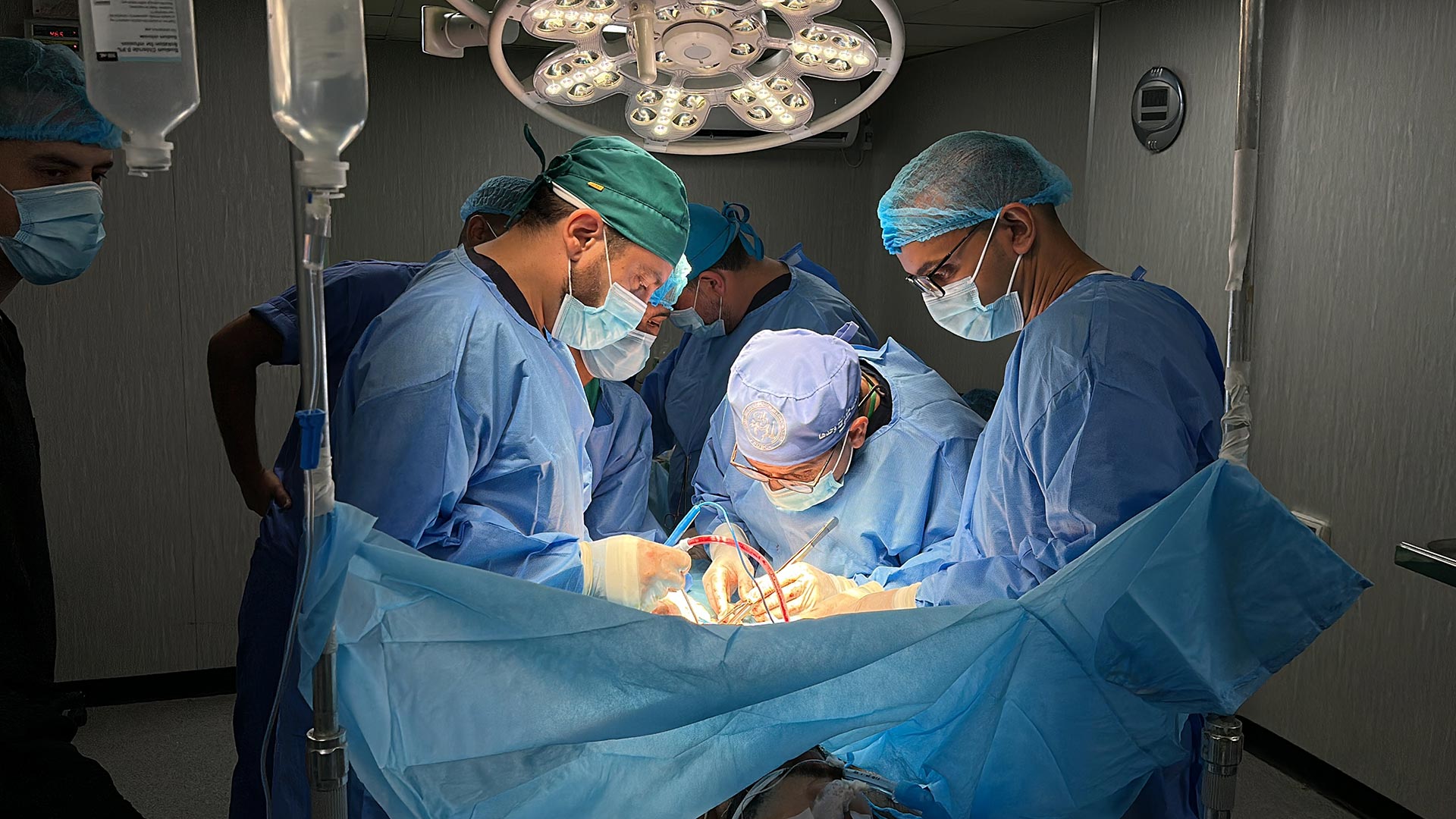 International EMTs performing a surgery in Public Health Hospital in North Gaza
International EMTs performing a surgery in Public Health Hospital in North Gaza
The scale of death and injury was an overwhelming burden that most health systems anywhere in the world would have not been equipped to bear.
When conflict overwhelmed Gaza's health system, the pressure on trauma care became almost unimaginable. In this episode, three experts who were on the ground speak with WHO: a national emergency medical team leader, a WHO EMT coordinator, and a WHO trauma surgeon. Together, they recount what it took to treat the injured — triaging patients amidst insecurity, transferring them from hospitals that were near active conflict, making impossible decisions in real time, and keeping care going when supplies, staff, and safety were all running out. From the story of one patient moved three times across a collapsing health system, to the role of the national emergency medical team in keeping Shifa Hospital functioning, this episode is human account of resilience to keep health care going.
Guests
Dr Thanos Gargavanis, WHO Regional Trauma Expert, WHO EMRO
Dr Motasem Salah, Team Lead National Emergency Medical Team (EMT) in Gaza, Shifa Hospital
Dr Heba Alnajjar, WHO Emergency Medical Team Coordinator, WHO oPt
Transcript
Egmond Evers (00:05)
Welcome back to the Frontline Shift podcast by WHO that looks at what it really takes to keep healthcare going in Gaza through coordination and deployment of emergency medical teams. I'm your host, Dr Egmond Evers, Health Emergencies Team Lead for WHO in the occupied Palestinian territory (oPt).
Luca Pigozzi (00:21)
And I'm Dr Luca Pigozzi, Acting in Charge of the WHO office in Gaza.
Egmond Evers (00:26)
During over two years of conflict in Gaza, healthcare workers have faced an almost impossible task managing a constant stream of catastrophic traumatic injuries in a healthcare system pushed to its limits.
Luca Pigozzi (00:37)
Since October 2023, nearly 172,000 people have been injured and over 72,000 killed. These figures are almost impossible to comprehend, for a health system already stretched beyond capacity, operating under bombardment and with dwindling supplies. The scale of death and injury was an overwhelming burden that most health systems anywhere in the world would have not been equipped to bear.
Egmond Evers (01:07)
In this episode, we explore how health facilities responded to traumatic injuries under relentless pressure, how care was delivered despite severe shortages of supplies and staff, and what is being done to build resilience and ensure the health system can respond to future emergencies.
This is the Frontline Shift
Luca Pigozzi (01:28)
With us today, we have Dr Motasem Salah, Team Leader of the National Emergency Medical Team (EMT) in Gaza, deployed at Shifa Hospital. The National Emergency Medical Team was founded in 2021 and has been deployed in Shifa Hospital since September 2024 to support the delivery of emergency care. We have also Dr Heba Alnajjar, WHO Emergency Medical Team Coordinator based in Gaza and part of many critical missions that WHO conducted during the conflict to support hospitals and health systems.
Egmond Evers (02:02)
And Dr Thanos Gargavanis, WHO Regional Trauma Expert and Surgeon who was based in Gaza running WHO missions and operations during the peak of the crisis.
Thanos, you were part of the response from the very beginning and carried out some very critical missions. Tell us about what you saw about the scale of the human tragedy and how the health system coped.
Thanos Gargavanis (02:23)
Hello, everyone, and thank you very much for having me. When this dreadful crisis started, the number of casualties and fatalities that we saw were exceeding anything that we had seen before. The health system in Gaza was already in a difficult situation before this crisis. The World Health Organization had been investing for quite some time to establish an effective trauma system in Gaza. And the results were that we had established a sustainable trauma pathway, meaning that there was a way to make sure that every trauma patient from the point of injury to rehabilitation would be following a precise pathway, meaning that there was somebody that would be taking care of him in the first phase that was pre-hospital care. They would be taken either to a trauma stabilization point or to initially primary health care center for the initial stabilization. And then based on the severity of the injuries, he or she would be referred to a designated hospital or not.
All this work was of extreme importance when this crisis started, because there was an institutional memory and the systematic capacity made everything easier, not easy, easier to respond. During the first moments of all this crisis, when we first set foot on the ground, the images that we have seen inside the hospitals and inside the improvised receiving facilities were really devastating. We have seen people lying on the floor with blood gushing out of open, devastating injuries. We have seen extremely overwhelmed and heroic medical personnel and nursing personnel who were trying to do their very best with the limitation of resources available. We have seen families bringing their beloved ones mourning for the death and for the loss of others that they could not save on time. And we have seen a system that was trying to reinvent itself while the disaster was ongoing.
Luca Pigozzi (04:48)
Thank you, Thanos. What you just described is truly devastating.
Egmond Evers (04:52)
As of January 2026, there have been more than 3400 serious injuries to the head, neck and spine. Over 22000 limb injuries. More than 5000 amputations, over 3000 burns and over 8500 other major injuries. Each one of those numbers is a person. A life changed forever.
Luca Pigozzi (05:15)
Thanos, back to you. You were on the ground helping to get medical supplies to hospitals and transferring patients from one facility to another for the safety or appropriate care. Throughout the conflict, are there any particular cases that you remember and you want to share with us?
Thanos Gargavanis (05:35)
Each and every case has its own story, and I wouldn't like to be unjust to others. However, the case that always comes to my mind and the effort that the World Health Organization, along with partners and the existing health system, invested to make sure that we save lives — brings me to a patient of around 40 years old. A man that we had to move three times as the front of the conflict was changing.
The man had sustained devastating spinal column injuries in November 2023 in Gaza City. He was moved to a nearby hospital, Al-Ahli Hospital, where unfortunately there was not enough equipment and supplies for a proper neurosurgical stabilization of the spinal column, and the patient was waiting for a referral to a safer haven and to another facility where he could be operated. That was the first time that he joined one of the WHO missions in November 2023, when we moved him, and took him from Al-Ahli Hospital to European Gaza Hospital.
From European Gaza Hospital before Christmas, the patient had to move again and went to Nasser Medical Complex because, again, there was extreme lacking of supplies and equipment and the surgical personnel could not deliver what in other circumstances could should be delivered. Finally, the third time that we have seen the same patient was in February 2024, when the front was moving that fast that Nasser Medical Complex got engulfed in the conflict. Then, in a series of four consecutive missions, the World Health Organization, along with PRCS and other UN agencies, we relocated the last remaining 87 patients that were remaining in the hospital.
It still strikes me that one of these patients was this man. The man that had initiated his treatment, travelling from Al-Ahli Hospital in Gaza City, then to European Gaza Hospital and then ended up again in Nasser Medical Complex. And unfortunately, he was never able to be properly treated and properly operated because we were never able to source the necessary equipment and supplies that were needed for the stabilization of his fracture.
Finally, the patient ended up in one of the field hospitals where another suboptimal solution was chosen. He was treated in a more conservative way and with a different surgical technique to stabilize the spinal column. However, what relieves me is the fact that the man has remained able to move his legs and toes, because what we were afraid was that eventually he would be paralyzed from the waist and below for life. And it still strikes me that none of his kith and kin were able to be with him during all this trouble.
Luca Pigozzi (09:13)
Thanos, what you have described is, sadly, I'm sure, the story of countless patients injured during this conflict, people forced to move from place to place and unable to access the care they needed.
Egmond Evers (09:26)
Heba, like Thanos, you've been right in the thick of it in Gaza. You've been doing critical missions, triaging patients, and making decisions about patient referrals. Can you take us through the process a little? What did it look like on the ground, and what were some of the most difficult calls you had to make?
Heba Al-Najjar (09:43)
Thanks for having me on today's episode. I want to talk about something that defined much of our work during the crisis in Gaza, actually moving patients out of the hospitals that were no longer safe or functional, some facilities had been attacked. Others were located in areas under active evacuation orders or close to hostilities. Our role was not only just coordination. We were on the ground transferring critically ill patients and facilitating where they could continue receiving care. Let me share some of what that looked like during this time. One patient we transferred had burns covering 70% of her body. She had no family with her, no companions at all. We moved her in an ICU ambulance, but at the checkpoint, we were held for a significant wait. As medical team, we were carefully managing her sedation, keeping her stable and keeping her out of pain until we could get her to another ICU and hand her over to another medical team. The hospital had also become shelter. Entire families were living inside the buildings and in the surrounding areas, all of them were under evacuation orders. Many had no place elsewhere to go. When we arrived at the hospitals, many of the families were approaching us asking us if we can move them as well with no other way out. It was a truly desperate situation. Some transfers required a lot of real time decisions. Required a lot of medical care during the time of transferring to patients, I remember one case with CADUS. The convoy was ready to move patients loaded, and all of a sudden one of the staff member came to us. This staff member was telling me that the patient had just started to be desaturated, and had a chest tube with him, and then it was a decision, shall we just leave him in an empty hospital, or we take the decision and we accept the risk and just move him with us? We made the call to take him with us, and if he got deteriorated during the transportation in the road, we would stop the convoy, stabilize him, and move again. This was one of the most difficult decisions we took in the field. And then there were a lot of hospitals like themselves. Those hospitals was not able to receive patients as there is no clinical stuff remaining inside those hospitals. We would arrive and find patients scattered all over inside the hospital, in different wards, different floors. We didn't have any staff member who can hand over the patients to us, no documentation, and sometimes very, very little paperwork with the patient. We had to go through the building, looking for the patients, trying to find out where they are sitting, and assess them, stabilize where needed, and then put them together and try to collect them and put them inside the ambulances and find out whatever paperwork would be available with them and can help, because when we arrive to the other hospital, when they should be receiving the patient they need, something to work with and to start, at least to know what this patient had in the other facility before. Actually, none of it was easy at all. We were not only dealing with injuries that very complicated and very complex from all kinds, but also many hurdles delaying and getting patients the healthcare that they needed.
Luca Pigozzi (13:20)
Thank you so much, Heba. What has the role of the emergency medical teams been in providing surge capacity and building resilience of the health system during the emergency response in Gaza?
Heba Al-Najjar (13:32)
Since the EMT program was officially activated in December 2023 emergency medical teams have become an essential part of the healthcare system in Gaza, working shoulder to shoulder with the local healthcare workers and trying to keep it functional under extraordinary pressure. The numbers speak to the scale of the effort that the EMTs conducted, starting from December till now, more than 44 partners and organizations deployed EMTs regularly, more than 56 teams deployed, and more than 4 million consultation were achieved since the start of the crisis. But the numbers only are telling part of the story. It's not telling everything. Many Palestinian health care workers couldn't reach even their facilities and where they are working, they were displaced. Some of them were killed and some forced to leave the country, searching for the safety of their families and for their children. EMT stepped into this gap and tried to support as much as possible, but it was never about replacement. It was all the time about how we can work together to support the healthcare system. It was always about integration and partnership. They were also not only surging and trying to provide services, but also tried to train the local staff member, transferring the skills to them and trying to build their capacity, including inside emergency departments, inside the operation theater, everywhere, where they were working together in the most difficult conditions, even during mass casualties, they were trying to make them aware how to deal with the situations in a proper manner. Actually, what helped us to have a successful response during the last period was the strong coordination framework behind that between all of the EMTs, Minister of Health, local partners and other international NGOs, different organizations deployed and were working together inside. All of them were sharing a same goal, which is ensuring that patients have access and receiving quality of care, and all of them were trying to ensure the minimum standard, regardless all of the circumstances we were working under. One of the most important lessons learned during the crisis here inside Gaza, it's about the critical importance of building national capacity. There were times when international teams and organizations couldn't get in and didn't have access. Some specialized teams were denied access completely. The reality that we understood while we are working that we need to focus on building national EMTs, and actually we succeeded in building two national EMTs during the last period. Teams can completely deploy by themselves, sustain longer and operate independently under whatever circumstances, under all of the risks. When international support maybe can be delayed or blocked so nationals can take the lead and working and supporting their healthcare system. Currently, in those days, international EMTs are playing a mentorship role. They are trying to equip and train all of the national emergency medical teams with all of the tools and all of the equipment, and providing all of the technical guidance for them, and trying to hold the line on their own until additional so the national EMT can hold the line by their own and try to provide the needed services until additional support can come and arrive.
Egmond Evers (16:58)
Thanks, Heba. Dr Mutasem, could you tell us a bit about how the national EMTs have been helping to manage the emergency caseload at Shifa Hospital?
Motasem Salah (17:08)
In April 2024, Shifa Medical Complex, the largest tertiary health care facility in Gaza Strip, was heavily damaged and effectively put out of service during the war. The hospital was left unable to function as a medical facility. Most buildings and equipment were destroyed. Complete destruction of all operation systems and the hospital could no longer operate normally as a hospital.
In response, Ministry of Health worked in rehabilitating the outpatient clinic building to serve as an emergency department. In 2024, through the EMT and with the support of MoH and WHO, Shifa Medical Complex was reopened with the capacity of thirty beds, two operation rooms, intensive care unit beds, and laboratory services, and severe cases needing admission were referred to other hospitals.
A national EMT played a vital role in managing emergency and trauma caseload. The medical team at Shifa Hospital implemented an effective triage system to control the flow of patients. Triage was conducted outside the emergency department to manage the cases efficiently.
The EMT improved the emergency response capacity with support of WHO. We trained all the staff in primary health care and in emergency departments.
Luca Pigozzi (18:42)
Thank you very much, Dr Mutasem. In fact, the dedication of the national EMT in Gaza is priceless, and the restoration of emergency care at Shifa Hospital was just due to the deployment of the national EMT. So again, big thanks to you and to the national team.
Thanos, let's get back to you. As the work on rehabilitation and recovery of Gaza proceeds, what are the key needs and challenges in ensuring a resilient health system that can cope with an influx of casualties?
Thanos Gargavanis (19:15)
What everybody needs to understand here is that the World Health Organization stepped in to address the needs that came out of this conflict, because it was really the last resort. The World Health Organization stepped in to provide supplies, to provide medication, to support and coordinate international emergency medical teams, mentor, and do the very best so that the national emergency medical team delivers at the best of their capacity and eventually try to address different gaps at different levels of care.
However, we are far from over right now. The system is struggling to get back to where it was. And I hope that with the steady flow of supplies and medical equipment and surgical equipment, we will never see again cases that ended up getting amputated because of the inability of the entire health system to save the limb. When we're talking of saving a limb, we all have to understand that this is not something that can be attributed to just one action. You must be having adequate care in the first step when you receive the patient so that you decrease the possibility of future infections. You must be having adequate nursing capacity. You must be having enough food so that the patient is properly nourished and is able to respond to the needs of his healing process. You must be having operation theatres that are clean and can be used to manage very complex injuries without exposing further the patient to danger.
Unfortunately, during the peak of this war, we have seen numerous times that patients had to be subjected to amputations because the system was not able to provide all the necessary means to save these limbs. I truly hope that with a joint effort from the international community, other health partners and the World Health Organization, the system will be able to sustain the reconstruction — that it's a long process, a process that requires commitment not only from the health system but from the community as well, so that the patient that goes through this process gets supported all along the way. And eventually we will be having people that, after their injuries, will be able to return to their community as equal members that are able to go outside, support their families, work, and have a life that resembles normal life as much as possible.
More investment is needed. More commitment is needed. Open passages are needed and a sustainable medical evacuation for those that cannot be treated inside Gaza is also needed.
Egmond Evers (22:30)
Thanks a lot, Thanos. As you've mentioned, Gaza will really need continued support to be able to transition to recovery and reconstruction. What we've heard today is a testament to the courage of health workers who would not stop, of patients who didn't give up, and of a health system that, despite everything, refused to collapse.
Luca Pigozzi (22:49)
The road to recovery in Gaza is long and the needs are immense. But as today's conversation makes clear, the commitment to rebuild and to do so in a way that prepares for the future remains as strong as ever.
Egmond Evers (23:03)
To everyone working on the front lines of this crisis, inside hospitals, in the field and behind the scenes, thank you. This has been the Frontline Shift. These are your hosts, Egmond and Luca, signing off.
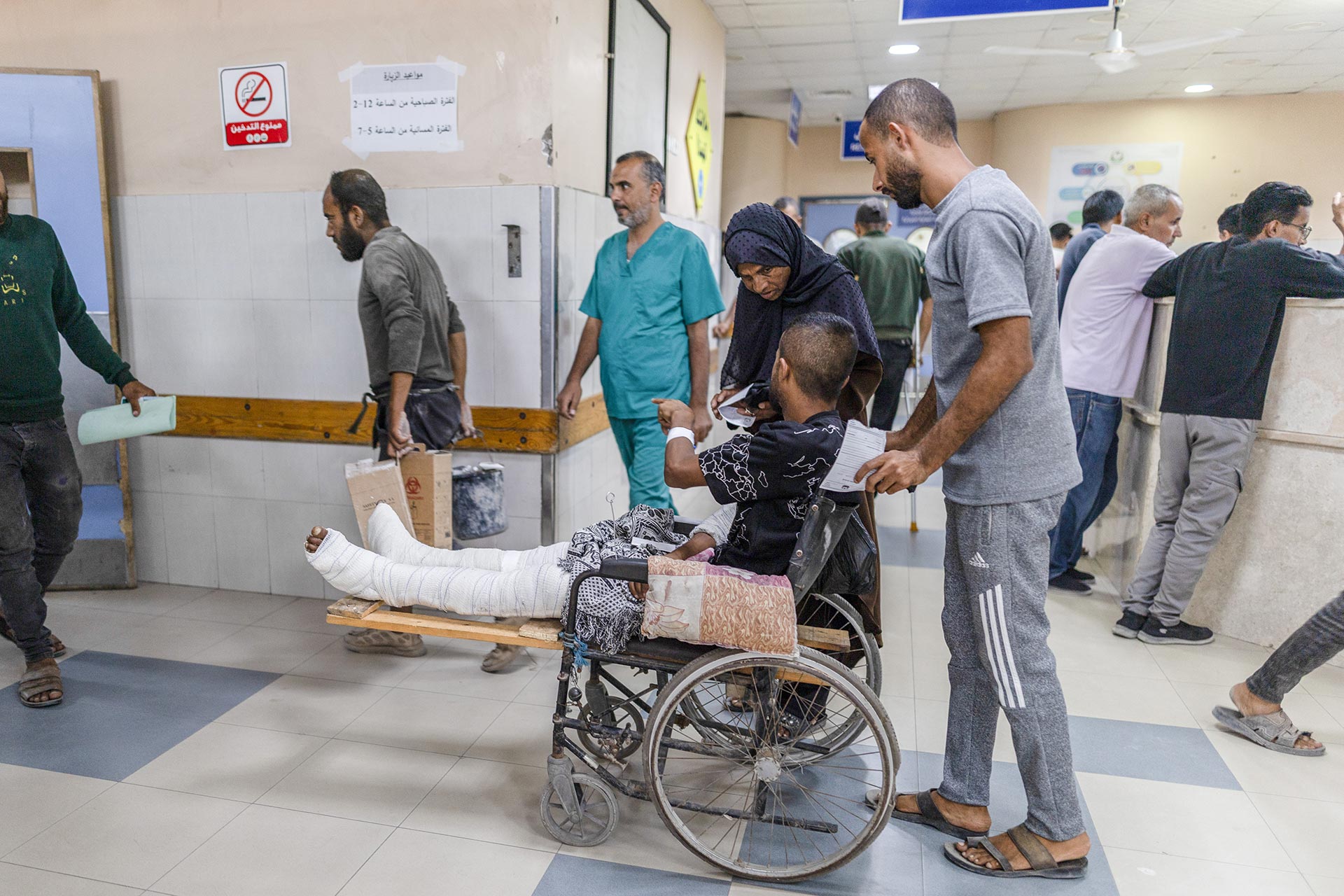
Episode 3: Delivering Primary Healthcare in Gaza
 A health worker examines a child at a primary health care centre in Gaza.
A health worker examines a child at a primary health care centre in Gaza.
I can't emphasize enough how hard it is to operate and provide good healthcare or even basic healthcare or any level of healthcare with such limited resources is incredibly, incredibly difficult.
After two years of conflict, only half of Gaza's primary health care centres remain functional. In this episode of the Frontline Shift, health workers from UKMed — an Emergency Medical Team working in coordination with WHO in Gaza since January 2024 — share what it has taken to keep primary health care going under relentless pressure. They discuss the immense challenges of operating with critical supply shortages, maintaining continuity of care for displaced populations, and reaching communities in areas with little to no functioning health infrastructure.
Primary health care is the entry point into the health system. Keeping it functioning is not just about treating illness, it is about restoring trust, dignity, and the foundations of a resilient health system for the people of Gaza.
Guests
Jay Matthews, Operating Department Practitioner, UK-Med
Mandy Blackman, Health team Lead for the North of Gaza, UK-Med
Transcript
Egmond Evers 00:05
Welcome back to The Frontline Shift, a podcast by WHO that looks at what it really takes to keep healthcare going in Gaza.
Luca Pigozzi 00:12
And howw, after two years of conflict, emergency medical teams supported and coordinated by WHO remain an integral part of the health system, rehabilitation and reconstruction efforts in future.
Egmond Evers 00:25
I'm Dr. Egmond Evers, Health Emergencies Team Lead for WHO in the occupied Palestinian territory.
Luca Pigozzi 00:31
And I'm Dr. Luca Piggozi, acting in charge of the WHO office in Gaza.
Egmond Evers 00:35
Over the past two years of conflict in Gaza, the health system has been under immense pressure. Hospitals have been damaged and have become non-functional. Medical supplies remain insufficient and healthcare workers are working under extremely difficult conditions.
Luca Pigozzi 00:49
In this context, primary health care centers have become more important than ever. They are often the first point of contact for people seeking care. When they are functioning well, they can treat common illnesses early, manage chronic conditions and support maternal and child care before problems become emergencies.
Egmond Evers 01:06
By providing care close to communities, primary health care centres help prevent overloading of hospitals and ensure that people can access essential services even when hospitals are not accessible.
Luca Pigozzi 01:16
In this episode, we are taking a closer look at the role of primary health care and the support from the emergency medical teams in this domain in the Gaza response. How these centers help sustain the health system and what it takes to keep them running.
Egmond Evers 01:34
This is the Frontline Shift.
With us today we have two colleagues from UKMED, Jay Matthews who is an operating department practitioner and Mandy Blackman, health team lead for the north of Gaza, speaking from Gaza. They have been working with UKMed as part of the WHO Emergency Medical Teams initiative. UKMed has been supporting the health response in Gaza since January 2024.
Welcome.
Jay Matthews 02:01
Hi, thanks for having us.
Mandy Blackmon 02:02
Hello, thank you for having us.
Luca Pigozzi 02:05
In Gaza, primary health care centers have faced many of the same challenges as hospitals, limited supplies, shortages of local health care workers, staff working around the clock, access constraints and ongoing security threats. Despite all these difficulties, health workers have continued to find ways to deliver care to their communities.
Egmond Evers 02:26
Currently, only 51% - that's 107 out of 209 primary healthcare centers that existed in mid-2023 are functioning in Gaza. Over the last two and a half years, insecurity has forced several clinics to suspend operations or relocate to continue serving displaced communities.
Luca Pigozzi 02:43
However, due to population displacement and their proximity to dangerous areas, some locations remain severely underserved.
Egmond Evers 02:53
North Gaza is a clear example. After months of siege, access restrictions and security challenges, the area was left without any functioning health services for a long period. While some clinics have since reopened, there are still no functioning hospitals in the area.
Luca Pigozzi 03:08
In the northernmost parts of this area, access to primary health care remains extremely limited. To address this gap, UK Med, together with WHO, has just established a clinic in Jabalia, the Al-Tayyeb Primary Health Care Centre, to help restore access to essential services.
Mandy, tell us why establishing this clinic is so critical right now.
Mandy Blackmon 03:31
Following our assessments up in the north, you can see that the area was very desolate. There weren't that many people living there at the time, and that was in November, but since then the population has increased. So primary health care is an integral part of the community where everybody lives and the clinics that are based within that community offer a place of proximity for people to access the services and fundamentally it prevents people either having to travel great distances, which is so difficult in this context, and prevents admissions to the other hospitals, to the larger hospitals around, so it doesn't sort of impact services.
Egmond Evers 04:06
UK Med has a lot of know-how on providing primary health care in difficult settings from Gaza and many other contexts. What can you tell us about the challenges in running primary health care in Gaza? What does it take?
Jay Matthews 04:18
So running a primary health care center in Gaza, it takes a whole variety of different support structures and efforts from a whole team. There's obviously one of the biggest problems in Gaza, uniquely, it's getting supplies in. So getting supplies to our facilities to treat people, to provide basic care for wound dressings and wound management for obstetric and gynocare, to normal injuries that have happened through the war itself, to getting pharmaceuticals like drugs, antibiotics, painkillers, really difficult to get through and get into place. And so rationing those through the community can be really difficult. So making sure the community is aware of these limitations so they know that we're doing the best we can for them through RCCE (Risk Communication and Community Engagement) outreach is really important. So that's probably the first and one of the most difficult things is managing the supplies, building materials to make new structures if you're going to deliver new services when you identify what people need as you integrate and as the dynamics of the situation change. So going from conflict into a ceasefire, what the community needs, as PHC (primary healthcare center) dramatically changes. So adjusting for that needs more logistical input, new WASH input, new materials, and security reassessments. We need to look at staff, both internationally and nationally. There's a huge amount that goes into keeping a PHC to maintain basic health needs for the people up and running.
Luca Pigozzi 05:56
Thank you, Jay. You mentioned the term RCCE. Just to elaborate for our listeners, RCCE is Risk Communication and Community Engagement, which refers to ensuring communities are well-informed about health risks and issues, and know how to protect themselves or what is being done to support them. You have worked in Gaza for some time. What are some of the most common cases you see and what does the typical caseload look like?
Jay Matthews 06:28
Yeah, so we see a lot of variety, but the main stay of cases that I see in November and December when I was managing the type one facility at Darabella was upper respiratory tract infections and a lot of gastric illnesses. They were our big two that we saw coming in. That obviously puts a lot of strain on the staff because they had to try and make progressive treatment plans to really limit the antibiotics because we had such a short supply. As an idea, I think it was something in November, December, it was something like 55, 56% of all pharmaceuticals had ruptured, so they're at 0% so we don't have them. So as an idea, We have very, very low supplies of drugs and materials for wound dressings and bandages and swabs were ruptured at like 65%, maybe 70% I think it was. So in terms of caseload, we're seeing when it was conflicts, it was about 700, 800 patients a day. And as Mandy said, as people were allowed back into the North, we saw that start to spread. So that went down to about half the patients, about 350 patients a day coming in to the primary health care centres and they were sitting for a variety of cases, mostly respiratory and gastro. We had other clinics in our facility. We had obstetric and gynecology and we had sexual and reproductive health being seen by our doctors there, also assisting with family planning. We have a lot of physiotherapy which went from only seeing a couple of patients a day, say three or four, working up to 20 as people readjusted to what facilities were available and what care was being provided. So we went from offering that twice a day to offering it six days a week. So it went up quite a lot. So in terms of caseload, we're seeing a lot of changes in the caseload, and I'm sure that if I go back in April, I'll see again another change in the caseload. But a lot of that stuff, we need a lot of support from the RCCE, so the outreach into the community, to educate people on how to manage their WASH, how to manage to mitigate against things like the flu, what symptoms will look like for certain diseases that pop up. Sometimes you'd see things like hep A start to track around the country. So we would then make sure the community understood what that looked like and made sure that we had the best resources possible to treat anybody that did have that and know where they should be going as well. So it's a big team solution to make sure that patients go to the right places within the country with minimal travel. As Mandy said, traveling in Gaza is actually incredibly difficult.
And it's not only difficult, it's really dangerous as well.
The roads are not safe.
And so I think that for the people to be moving on dangerous roads, they really need those PHCCs.
A huge, huge difference to have the primary health centers and the Type 1s in lots of
communities close to where they are to reduce all that risk to the people that are already facing so much trauma and danger.
Egmond Evers 09:37
Thanks, Jay.
Luca Pigozzi 09:38
I just want to quickly come in for our listeners and explain Type 1 and Type 2 as Jay mentioned, because I'm sure that these terms will come up again. Type 1 refers to primary healthcare clinics offering basic outpatient services, essential health consultations and preventive care serving as first point of contact with the patients. Type 2 instead refers to fully functioning field hospitals.
Egmond Evers 10:11
Over the past two years, security constraints have compromised access to healthcare. Under these circumstances, the primary healthcare centers have played a critical role in offering essential medical services to the community. Mandy, can you tell us a little bit about your experiences in this regard? Are there any examples that stand out from your work with UK Med?
Mandy Blackmon 10:29
Yeah, so with the restricted access to all healthcare services, obviously the impact for the primary healthcare service increases as it does internationally when these things happen. I think definitely the doctors and the nursing team are seeing more cases of injuries where maybe the wounds have been left for so long and that their healing has been impaired. What would have been a fairly simple wound now takes greater resources, greater lengths of time and the facilities for healing are less and with the reduced equipment that we have at our disposal, the lack of nutrition among the people of Gaza impacts upon their ability to heal, where we've got respiratory diseases especially coming through the winter where we see our peak and then as the weather changes going into the spring again, it's the medications we have to treat those patients, that can often exacerbate the disease. They can't maintain their normal levels and then we need to find the resources to treat them.
Luca Pigozzi 11:30
What were the working conditions like for health workers in primary health care centres during the peak of the conflict?
Mandy Blackmon 11:38
So working conditions obviously most of us are working at pre-fabricated buildings or tents. So obviously impacted by all the seasonal changes that are around us, like in cold environments with many of our medications and many of the equipment, just getting the fundamental equipment that we need is restricted. We don't have access to the resources that we would like in order to treat people. So a lot of the time we don't have the analgesic to give, we don't have the simple wound dressings to give. And this impacts upon the emotions of the staff as well because they're there, they want to do the jobs that they're there to do, that they're trained to do, that they're highly skilled to do and that are restricted in what it is that they can provide.
Jay Matthews 12:20
If I could add on top of that as well, like when we have patients come into the Type 1 that require further care because they can't get to a hospital, we would see that quite regularly. We had patients with severe asthma, which is like a respiratory condition and they would have to be treated in an emergency setting in a type 1, which is not what we'd normally do. But because they can't get to the place they need to go because of infrastructure collapse, because of the danger on the roads, they came to us first because we're closest to them. And we'd often see patients come in that clearly needed, as Mandy said, had worsening wounds from not being able to eat and drink normally and being malnourished. And so their wounds delay and then they get infected. They come to the type 1 because they can't get to the hospitals or the hospitals are so overwhelmed that they send people away because they just can't simply manage them as well. And so that became quite a loop system and it was really difficult to break that. We were lucky, UK Med have multiple facilities, one is just type two. And so we could often refer to ourselves if we couldn't get the patient into a national hospital or a hospital nearby and we would organise the transfer themselves but you'd often have to see your nursing staff dealing with cases that were outside of their normal remit for work in a Type 1 facility for sure and you would see a lot of people with just awful wounds coming in at different times.
Mandy Blackmon 13:55
So just to add to that as well, so yes especially in terms of chronic wounds we're seeing people maybe have been discharged from hospital earlier than they previously would have, but the impact is on the services of the hospital. It's meant that as soon as patients are well enough to leave, then they leave. So they're attending the primary healthcare services with wounds that probably haven't been seen, as Jay said, by the staff. But what the primary healthcare services can offer, even with the limited resources that we have, is that we can see those patients on a regular basis and provide them with the reassurance that they need. So we could make alternate day appointments for the patient to come in so that they can receive that wound dressing. And although the traveling to the clinic is hard for many patients, and just that reassurance, just that continuity of care that their primary health care systems can provide, and was very reassuring to the patients. You've also got parents bringing their children in, and maybe just, you know, what we would term as just common empatigo, but here, due to the lack of sanitation, you can't access the medications that can often ravage the body of the child. And so again, what we can offer at the primary health care services is that daily viewing of the child, that they can come back for extended appointments so that we can keep an eye on them and make sure that they are getting back to full health.
Egmond Evers 15:20
Thanks, Jay and Mandy. As the rehabilitation and recovery of the health sector in Gaza starts, what are the key needs and challenges for primary healthcare and what work is being done to overcome these?
Jay Matthews 15:33
Yes, so a lot of these challenges we face are things that I mentioned earlier in terms of our supplies, materials, logistics, security staff, RCCE outreach. We are looking regularly at redefining what is needed in the areas. So as we have a ceasefire in place, we have then gone back out into the community as we see less trauma coming through, and we look at what are the community's needs, what do they need next, and engage with the community. You find out they need things like dental work, you know, non-tremical disease care, like diabetes, hypertension. They need more focus on ophthalmology, eyes, and they need more care on dermatology, psychosocial support. So understanding what their needs are is really crucial in making sure you can make the right steps forward in delivering that care and then figuring out do we have the space, do we need to build more building supplies in to build tents or structures to house the new healthcare needs of the community and where are we going. A lot of the constraint is we would offer lots more services in the community, PHCCs, but often we don't have the supplies to offer more services. That is one of the biggest problems. We often look to collaborate with other charities or workers in country, so they can use our facilities to deliver certain care. I know at the moment we're working on putting together a link with some ophthalmology, and I am aware in the North they're working really hard bringing dental clinics together. I think those are things that are really needed at the moment and it's just making sure that these services that could get put in place can be continued. So making sure we have a plan in place to make sure that we can continue to run those services because we don't need them for just a week. There's been a gap in healthcare for over two years now. So the people really have a huge backlog of needs and support that they need to be given. So a lot of planning, a lot of capacity building, making sure that the team's training fully understand what needs to be given when we start offering new services, what to look out for, how those services should be managed. And I think that we really try and look at a holistic approach to making sure that services that are given to the community can be continued are managed. But the big problems are keeping staff safe, keeping our own staff safe, international and national staff, getting the supplies in. I can't emphasize enough how hard it is to operate and provide good healthcare or even basic healthcare or any level of healthcare with such limited resources is incredibly, incredibly difficult. So yeah, when we're looking at our PHC, whether we're looking at developing one in a new area, whether we're looking at changes in the healthcare needs in the service areas we're already in, we're constantly looking at evolving the PHC and we're constantly monitoring and addressing these challenges in a sort of circular approach.
Mandy Blackmon 18:56
I can add as well, so looking at all the maternal services as well that the PHCCs provide and supporting the vaccination programmes so that we're capturing people when they need us the most and providing that healthcare which then leads fundamentally to a healthier population.
Luca Pigozzi 19:13
This has been a very insightful discussion. Primary healthcare is the entry point for the patients into the health system and so critical to keep it alive through the EMT work in these circumstances. So many people are still underreached and then more access to healthcare needs to be granted. As efforts to restore Gaza health sector continue, sustained donor support remains critical, along with unimpeded access across Gaza and the large-scale flow of humanitarian aid. currently constrained by the ongoing closure of most crossings into Gaza.
Egmond Evers 19:42
Strong primary health care is one of the foundations of a resilient health system. If care starts early on close to where people live. Health services can be accessed faster, more effectively and more equitably. It's been great to hear about the work being done to ensure primary health care remains at the heart of the recovery efforts.
Luca Pigozzi 20:06
Thank you all for taking the time, especially in between demanding shifts and to share your experiences and the work you are doing.
Egmond Evers 20:13
These are your hosts Luca and Egmond signing off.
 A mother and child receive consultation at primary health care centre in Gaza
A mother and child receive consultation at primary health care centre in Gaza









