Occupied Palestinian territory
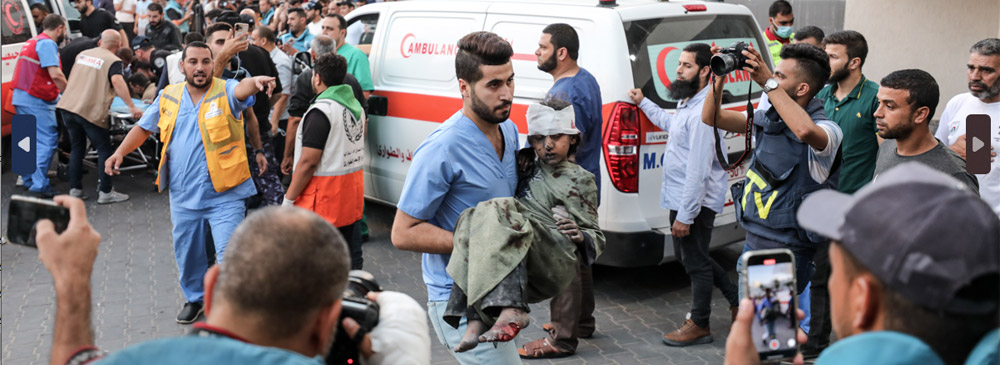
 Photo credit: Nicola Baldwin
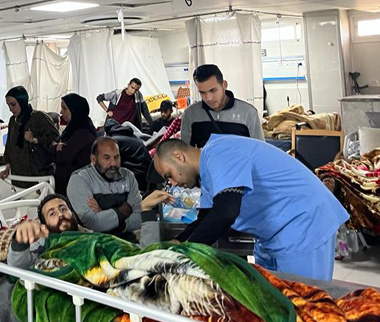
Photo credit: Nicola BaldwinHead of Office, World Health Organization, Office for West Bank and Gaza (oPt)
Rik Peeperkorn
email: This e-mail address is being protected from spambots. You need JavaScript enabled to view it
WHO oPt office
Othman Ibn Affan Street, 24 Sheikh Jarrah
P.O. Box 54812
Jerusalem
Tel: +972 (2) 5400595
Fax: +972 ) (2) 5810193
Email:
This e-mail address is being protected from spambots. You need JavaScript enabled to view it